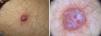
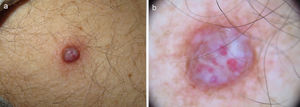
A 78-year-old man consulted for an asymptomatic cutaneous lesion on the external aspect of his left arm that had first appeared 7 months earlier. The lesion, which was firm and measured 15 mm in diameter, was papulonodular, dome-shaped, and erythematous-violaceous in color (Fig. 1A).
A, Firm erythematous-violaceous, papulonodular lesion on the external aspect of the left arm. B, Dermoscopic image showing whitish structures on an erythematous base, nonarborizing telangiectasias, vessels with a glomerular appearance, and a slight brown reticular pattern mainly on the periphery.
Arteriovenous tumor.
CommentPolarized light dermoscopy revealed the presence of whitish structures, a slightly brown reticular pattern mainly on the periphery, and vascular structures (nonarborizing telangiectasias in areas with a glomerular appearance), all on an erythematous base (Fig. 1A).
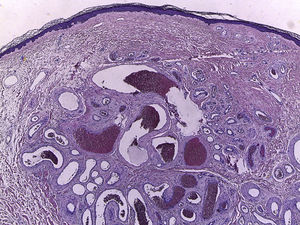
Given the clinical and dermoscopic characteristics of the lesion, the differential diagnosis was made with a vascular lesion, including arteriovenous tumor, aneurysmal dermatofibroma, and hypomelanotic nodular melanoma. The lesion was removed completely (Fig. 2).
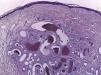
Histopathology revealed a well-circumscribed—but not encapsulated—proliferation comprising aggregated vessels in the dermis covered by a single layer of endothelial cells without atypia. Some vessels had a thick fibromuscular wall, with no definitive elastic lamina, and others had a thinner wall.
Arteriovenous tumor, or acral arteriovenous tumor, is a benign vascular tumor that is clinically difficult to diagnose. It usually manifests as a solitary, asymptomatic lesion mainly at acral sites, such as the head and limbs.1 It has been reported to appear on patch-like capillary malformations such as port wine stains.2
Histopathologically, the lesion is a well-circumscribed proliferation in the papillary dermis composed of multiple vascular spaces with thick walls interspersed with other spaces with thin walls. It has been suggested that this is a hamartomatous proliferation of the subpapillary plexus.3,4
A recent study of 39 cases summarized the dermoscopic characteristics of these lesions. The dermoscopic pattern most commonly associated with arteriovenous tumor was nonarborizing telangiectasias on a reddish background (72% of cases) in the absence of the lacunae that are typical of other vascular tumors. Furthermore, whitish structures and a slightly pigmented peripheral network were detected in 49% and 18% of cases, respectively.4
While it is true that dermoscopy can reveal vascular structures in aneurysmal dermatofibroma, these are observed at the edge of the lesion, probably in association with blood vessels of the surrounding stroma. This type of tumor has irregular spaces filled with red cells, although they lack an endothelial layer and, therefore, are not seen as central telangiectasias in dermoscopy, but as homogeneous reddish or bluish areas.5
In the case of hypomelanotic nodular melanoma, the relevant findings include a clearly atypical vascular pattern, mainly with irregular linear vessels and hairpin vessels, as well as milky red areas. In this context, pigment networks are unusual.6
In conclusion, dermoscopy could prove to be a useful tool for the diagnosis of arteriovenous tumor. However, the definitive diagnosis of this type of lesion necessarily requires a histopathology work-up.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Álvarez-Salafranca M, Fuentelsaz V, Cebrián García C. Tumor arteriovenoso: pistas dermatoscópicas para su sospecha. Actas Dermosifiliogr. 2021;112:359–360.