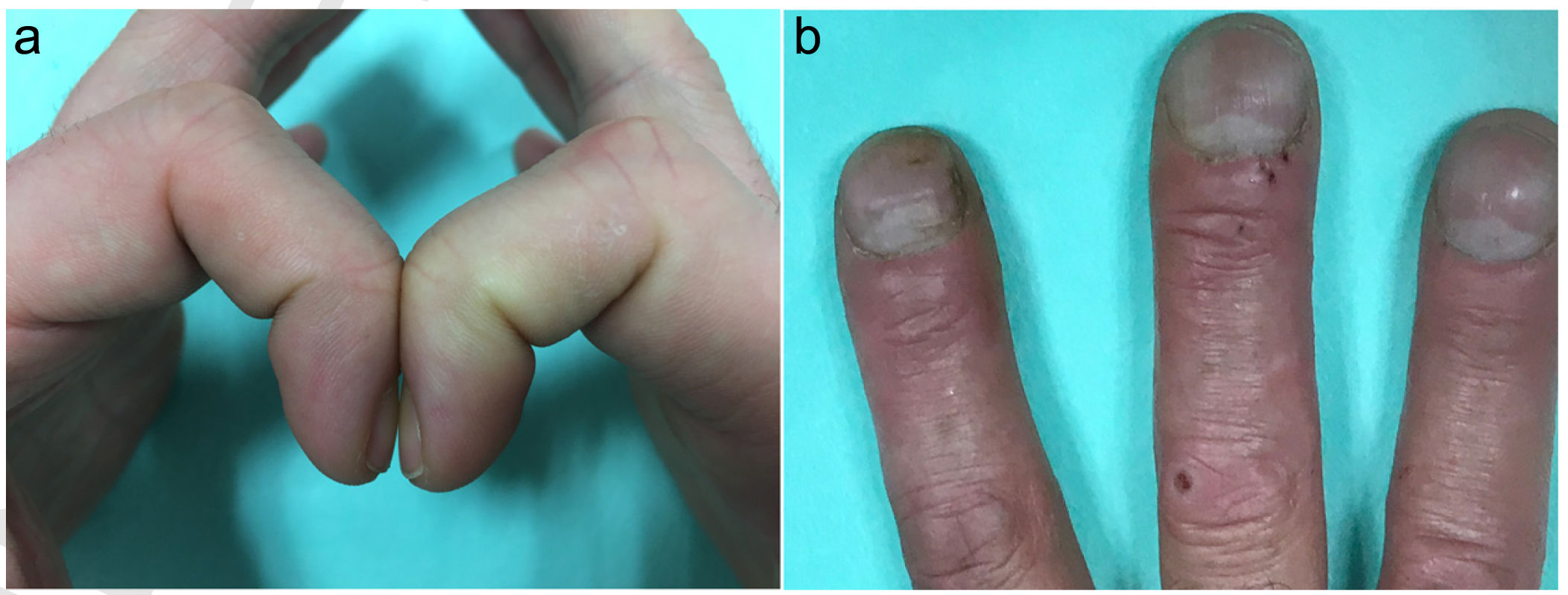
Digital clubbing refers to focal enlargement of connective tissue at the distal phalanges of fingers or toes. It is particularly prominent on dorsal surfaces and is often bilateral. Clinically, it is characterized by an increased Lovibond angle, which is the angle made by the proximal nail fold and the nail plate and normally measures 160° or less (Fig. 1a). In clubbing, it is larger than 180°, forming what is known as the Schamroth sign. The most common causes of digital clubbing are pulmonary (75%–80% of cases), cardiac (10%–15%), gastrointestinal (5%–10%), and thyroid (among others).
Ultrasound is a useful tool for evaluating the anatomy and structures of the nail unit as these show different degrees of echogenicity. In addition, Doppler measurements are helpful for assessing the vascularization of the nail matrix and nail bed. Ultrasound imaging has been used to characterize abnormalities observed in nail psoriasis and tumors of the nail and surrounding tissues, as well as nail changes in patients with autoimmune, infectious, and inflammatory diseases.1–4
In this report, we describe ultrasound findings observed in a patient with digital clubbing.
Case reportA 46-year-old male smoker presented with hand eczema of 2 weeks’ duration and paronychia secondary to onychophagia. The physical examination revealed clubbing (Fig. 1b), which the patient said had been present since childhood; he denied a family history of nail abnormalities and reported no pain or mechanical symptoms.
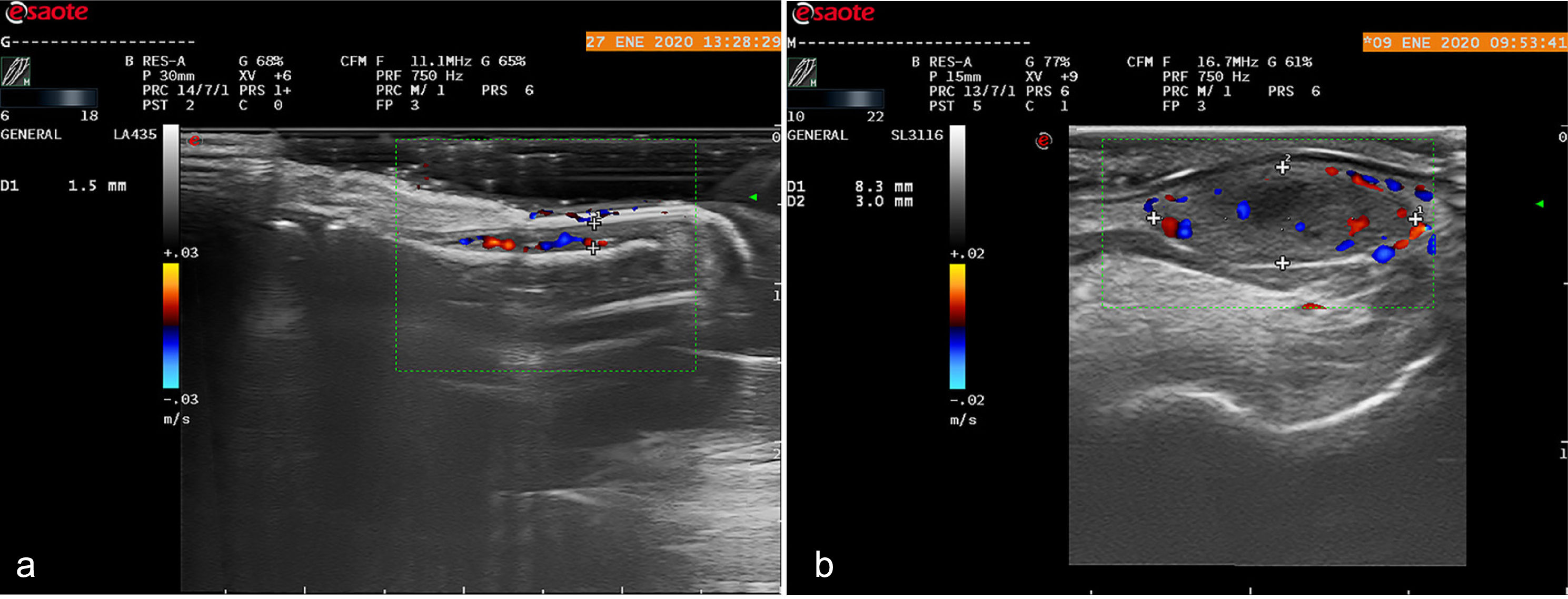
We studied the nail unit using high-frequency ultrasound with a 10–22MHz linear probe connected to an Esaote MyLab Class C system. The longitudinal view revealed an enlarged nail bed, with a diameter of 3mm (normal measurements are ≤2mm [Fig. 2a]), and increased vascularization through the full thickness of the bed. No alterations were observed in the bone surface of the distal phalanx (Fig. 2b).
CommentThe most widely accepted pathophysiologic hypothesis to explain clubbing is proliferation of vascular connective tissue due to platelets and platelet-derived growth factors (PDGFs). In the case of pulmonary diseases, it is assumed that circulating megakaryocytes cross from venous blood to arterial blood and are delivered to the extremities, where they release growth factors such as PDGFs. Normally, megakaryocytes do not fragment until they are trapped in the pulmonary capillaries, which is why clubbing is mainly associated with pulmonary diseases.5–7
Clubbing must be distinguished from pachyperiostitis, which is clinically characterized by subperiosteal bone neoformation associated with pain (hypertrophic osteoarthropathy), polyarthritis, cutis verticis gyrata, pachydermia, seborrhea, and hyperhidrosis.8,9 None of these features were observed in our patient. Ultrasound findings in pachyperiostitis include echogenic tissue surrounding the long bones, reflecting the presence of edema and inflammation. Doppler imaging shows increased vascularization on the surface of some superficial bony structures.10,11
Cutaneous ultrasound is an inexpensive, rapidly accessible, noninvasive tool for exploring the anatomy of the nail unit. In addition, it is useful for distinguishing between clubbing and pachyperiostitis without the need for ionizing radiation. Underlying disease must always be ruled out in such cases.
This is the first case in the literature to describe ultrasound findings in a patient with digital clubbing.
Conflicts of interestThe authors declare that they have no conflicts of interest.