The surgical treatment of periungual tumors is complicated by the risk of causing irreversible nail dystrophy. However, incomplete resection leads to a high risk of recurrence, and surgery must therefore eliminate the whole tumor while preserving the germinal cells of the nail matrix.
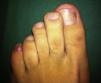
We present the case of a 31-year-old man who was seen in outpatients for a firm, pink, digitiform tumor of about 5 × 3mm that had been present on the fifth toe of the left foot for about 5 months (Fig. 1). The base of the lesion was beneath the eponychium but above the nail plate. The patient did not recall any history of trauma, and there was no family history or presence of other lesions suggestive of tuberous sclerosis. The clinical diagnosis was periungual fibroma and, as the patient reported discomfort due to friction against his footwear, it was decided to excise the lesion as an elective procedure.
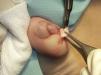
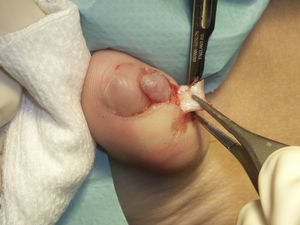
The operation was performed under local anesthesia with 2% mepivacaine, and a glove was tied around the proximal part of the digit as a tourniquet to provide a bloodless surgical field. Two longitudinal incisions were then made into the proximal nail fold, one on each side of the lesion. The proximal nailfold was then elevated (Fig. 2), exposing the whole tumor and enabling us to dissect and excise the lesion completely. During the procedure, special care was taken not to damage the matrix.
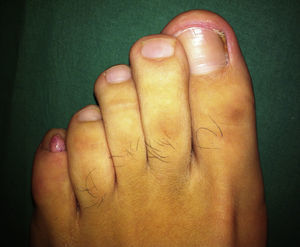
After resection, the flap was replaced to cover the defect and was sutured with interrupted 5/0 silk sutures, starting at the part closest to the cuticle. As the flap was narrow, the knots were placed outside its borders in order to prevent ischemia. Hemostasis was ensured by the application of Monsel solution with a swab onto the surgical wound, and there were no complications on removal of the torniquet. Finally, mupirocin ointment was applied and the area was covered with tulle gras, gauze, and an adhesive dressing. Histology of the surgical specimen revealed stromal fibrosis with vascular ectasia, compatible with fibrokeratoma. Follow-up at 1 year showed no nail dystrophy and no recurrence of the lesion.
Acral fibrokeratoma is a benign and typically solitary tumor. It is the color of normal skin and may be dome- or horn-shaped. This tumor may arise secondary to trauma.1 The term acral fibrokeratoma encompasses several entities, including acquired digital fibrokeratoma, acquired periungual fibrokeratoma, “garlic-clove” fibroma, and the subungual and periungual fibromas characteristic of tuberous sclerosis.2 These tumors should be excised when they cause symptoms or significant cosmetic problems.
Various surgical techniques can be used to resect these tumors, depending on whether they arise from above or below the nail plate. Lesions beneath the nail plate require partial or total removal of the nail. Lesions above the nail plate, on the other hand, can be removed by shaving followed by phenolization,3 carbon-dioxide laser vaporization,4 or, more usually, surgical resection after lifting the proximal nail fold as a banner flap.5
Surgical resection is usually performed under nerve block anesthesia. Two oblique incisions are made in the proximal nail fold, one at each end of the eponychium; the whole proximal nail fold can then be lifted to expose the lesion. This allows the base of the lesion to be evaluated and complete excision performed, preventing future recurence, without damaging the nail matrix.6–8 We used a simpler variant of this technique in which the 2 incisions were made along the borders of the tumor instead of making them at the medial and lateral ends of the eponychium.
It is important to note that this type of lesion has a tendency to bleed despite suturing, and correct hemostasis is therefore essential. The use of vasoconstrictors is not recommended in acral regions due to the risk of distal ischemia; a simple digital torniquet will adequately control bleeding. In addition, Monsel solution—a ferric sulphate solution that has a high local hemostatic potential—can be used to ensure correct hemostasis.9 Monsel solution is applied directly with a cotton bud or gauze swab after suturing.
We thus propose this technique as a useful alternative to wedge or punch excision. These other procedures usually provide poorer visualization of the lesion, with a higher risk of recurrence due to incomplete excision of the lesion or nail dystrophy if the resection is too wide. In addition, the technique described preserves the supralesional skin of the proximal nail fold, which reduces tension in the scar and achieves excellent cosmetic results. The banner flap is therefore a simple and very practical technique for small periungual lesions.
Please cite this article as: Yélamos O, Alegre M, Garcés JR, Puig L. Fibroqueratoma acral periungueal: exéresis quirúrgica en bandera. Actas Dermosifiliogr. 2013;104:830–832.