Herpetic geometric glossitis (HGG) is an infrequent manifestation of oral herpes simplex virus infection. Because it is a painful and incapacitating form of glossitis, a delay in diagnosis can lead to malnutrition and secondary infection due to an altered epithelial barrier function. While initially considered a disease found exclusively in immunocompromised patients, we describe a case of HGG in an immunocompetent patient who responded to systemic antiviral treatment.
The patient is a 30-year-old woman with a 12-month history of pain on her tongue and altered sense of taste. She had no relevant prior medical history and had given birth to a healthy boy one year before her consult. She described seeing lumps on the back of her tongue that seemed to grow progressively accompanied by increasing pain that sometimes made eating difficult. She also noticed hypogeusia and, more recently, dysgeusia. Recently, she noticed small ulcers in the inner part of her lips which caused further pain and discomfort. She had received treatment with oral nystatin but showed no improvement.
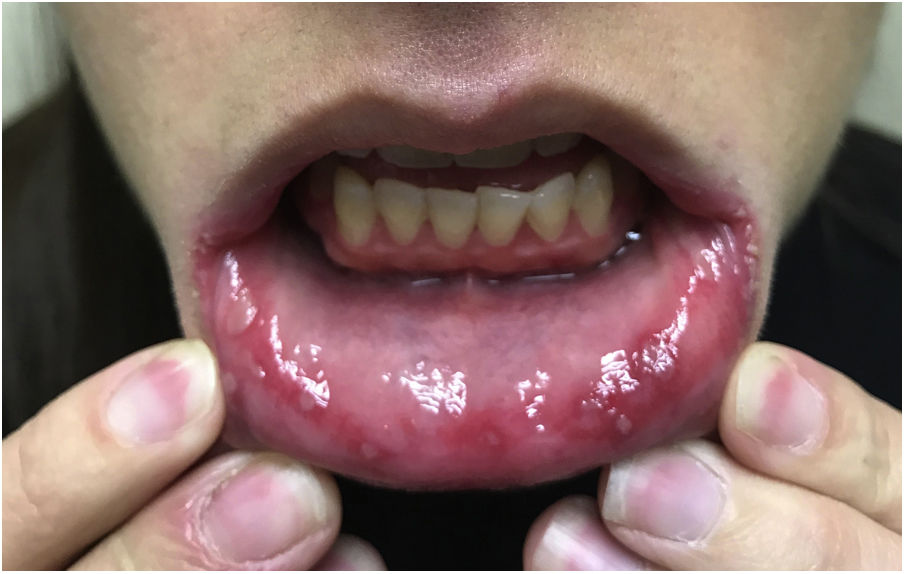
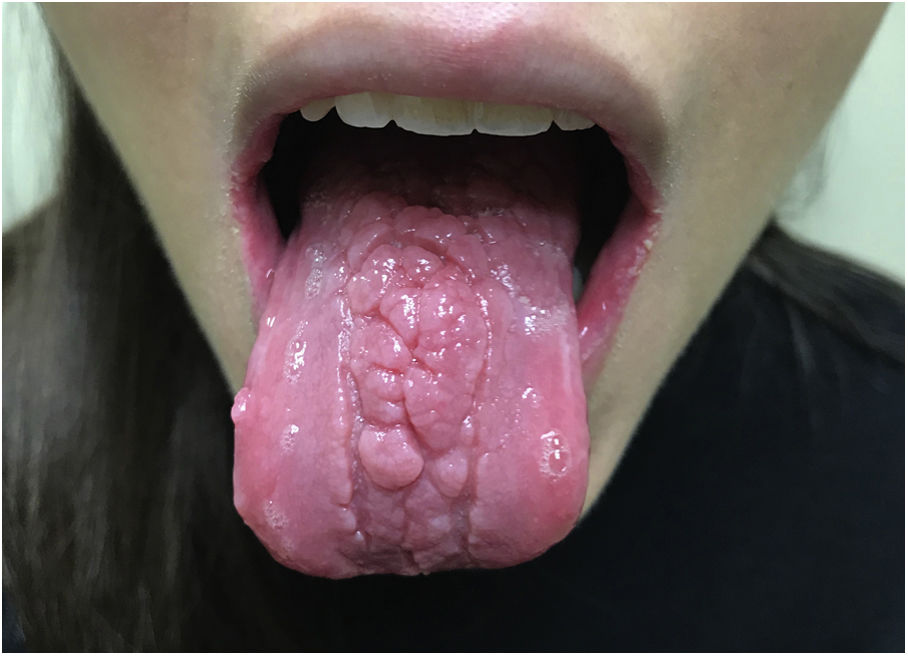
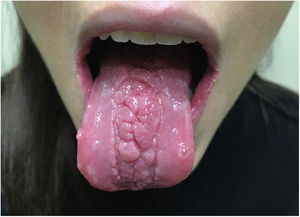
On physical examination of the oral cavity, multiple 2 to 5-mm shallow ulcers with an erythematous base were found in her lower labial mucosa (Fig. 1) and the lateral borders of her tongue. The middle third of the dorsum of the tongue had deep interlocking fissures that gave it a nodular appearance while the lateral thirds of the tongue had a smooth, atrophic appearance (Fig. 2). No associated adenopathy was found on examination.
A bacterial culture showed normal oral flora. A Tzanck smear of the ulcers showed numerous multinucleated giant cells. A second sample from the dorsum of the tongue showed the same cells in small numbers. Due to the presence of mucosal ulcers, deep tongue fissures and intense pain and a positive Tzanck smear, the patient was diagnosed with herpetic stomatitis and geometric herpetic glossitis. HIV test was nonreactive, complete blood cell count, C-reactive protein, serum immunoglobulins and blood chemistry were within normal ranges and antinuclear antibodies were negative.
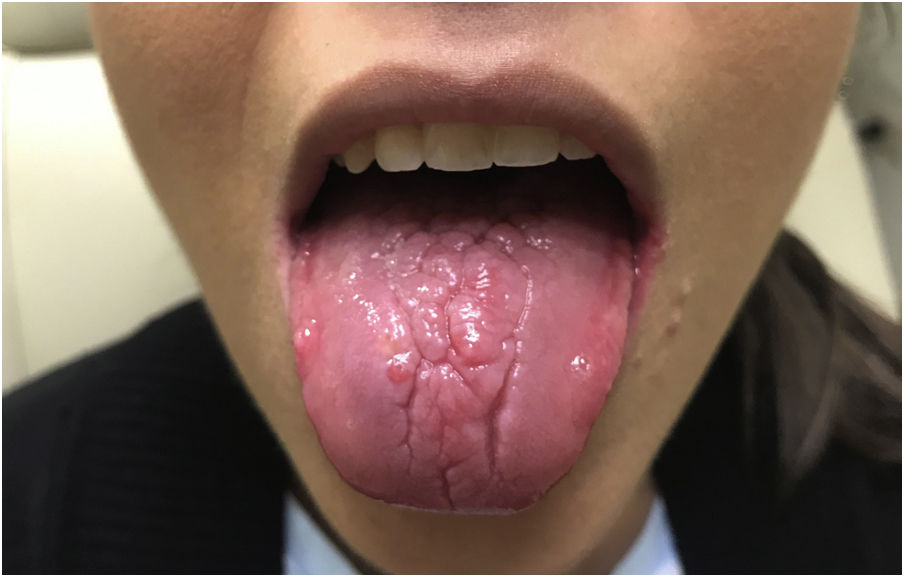
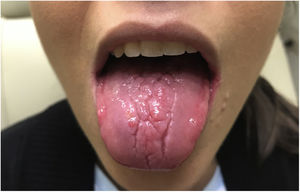
The patient was treated with acyclovir 400mg three times a day for 10 days. The lip ulcers, major fissures, pain and taste disturbances resolved completely after treatment (Fig. 3) while the dorsum of the tongue gradually returned to its normal appearance. The patient has not presented recurrences 12 months after treatment.
In 1993, Grossman et al. initially described 5 HIV-positive patients who presented with tender, geometric fissures in the central portion of the tongue; all patients responded promptly to oral acyclovir despite being severely immunosuppressed.1 Since then, a few more cases of herpetic geometric glossitis (HGG) have been reported, including a patient with no apparent immunosuppression.2–5 The fissures have been likened to those found in dendritic epithelial keratitis caused by HSV infection of the eye.6
Diagnosis is based on the clinical appearance of the dorsum of the tongue, the presence of associated pain or tenderness and evidence of viral infection. In this case, a Tzanck smear provided confirmation of viral infection but viral cultures and tissue histology are commonly used in hospital settings and may be warranted if clinical suspicion remains high despite a negative Tzanck smear test.7,8
The differential diagnosis for HGG includes fissured tongue, local trauma, mucositis due to chemotherapy, bacterial or fungal infections and recurrent aphthous stomatitis.1 The fact that it can mimic better known causes of glossitis such as oral candidiasis may explain why it is rarely diagnosed.
The condition usually responds to systemic acyclovir resulting in complete remission of symptoms and gradual disappearance of tongue fissures although a single case of acyclovir resistant HGG has been reported in a patient with acute myelogenous leukemia who responded to treatment with famciclovir.3 Antiviral resistance testing may be warranted if patients with confirmed viral infection fail to respond to treatment.8
HGG should be considered in the differential diagnosis of all patients presenting with mucositis or glossitis, especially if associated with pain or tenderness. A Tzanck smear can be included, along with other inexpensive and non-invasive tests such as a Gram stain, in the initial evaluation of these patients to rule out HHG and other common infections.