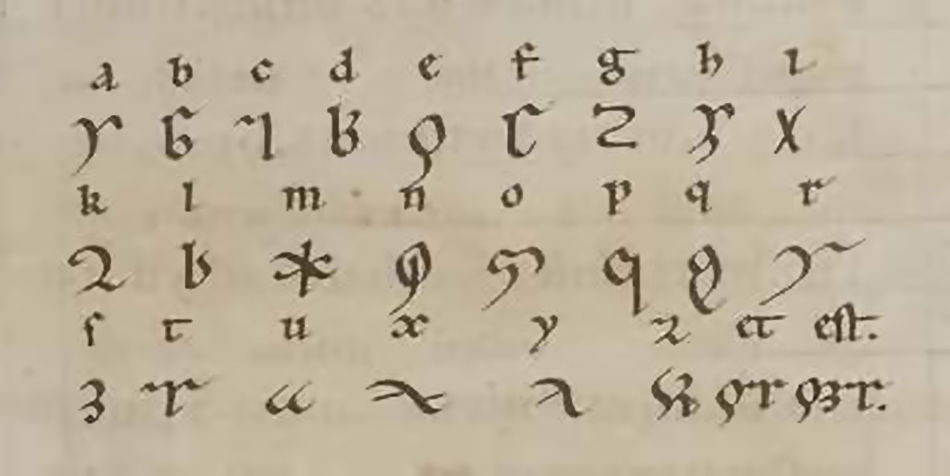The visionary nun Hildegard of Bingen (1098–1179), known as the Sybil of the Rhine, was a linguist, painter, healer, poet, and musician who dedicated a large part of her long life to the study of botany, human physiology, and medicine. Dermatologic diseases fell within her range of interests. The depth of Hildegard's work, her ability to observe nature, and the excellence of her music make it clear that the simple label of mystic applied to so many religious figures of her time is inadequate to cover the accomplishments of this many faceted nun, who merits consideration alongside learned Renaissance figures like Leonardo da Vinci and Galileo.
Hildegard was well-born and at the age of 8 years was called to a religious life.1,2 Her family brought her to the Benedictine monastery of Disibodenberg, where she was educated under the guidance of Abbess Jutta of Spanheim. At that time, the community comprised both nuns and monks,3 forming a type of mixed community that had been suppressed by Justinian, emperor of the Eastern Roman Empire, possibly in response to problems and scandals in convents. The practice nonetheless continued in Spain, Germany, and France during the High Middle Ages under theoretically strict rules governing how the men and women lived together. Benedictine nuns, known as the black nuns for the color of their habit, were among those who lived in such monasteries along with both monks and oblates, who were referred to as milites because they provided a certain degree of protection. It is clear that Hildegard's educators indulged her in allowing access to knowledge of copulation, conception, sexual relations, sexual dysfunction, and the female orgasm—which she described in detail (Appendix). It is possible that she had direct knowledge of what she described.
Hildegard had what were called visions from an early age, but it was not until 1141 that she decided to share them with others. She began by recounting them to her superior, Jutta, and the monk Volmar (Fig. 1), who served as her secretary and scribe until his death. Much has been said about Hildegard's mystical experiences, which were described and illustrated in great detail. It has been suggested that they might have been related to neuropsychiatric disorders that left her motionless for days or else the result of migraine aura, a symptom she was the first to describe.4 Her most enigmatic text, Lingua ignota, was written in a code that no one has been able to decipher (Fig. 2), and some have described it as consisting of psychotic neologisms.5 As the first constructed language recorded in history, it was a forerunner of Esperanto.
On the death of Jutta, Hildegard was elected abbess, but she later built her own convent in Rupertsberg, near Bingen. While head of that community, she continued to write with the assistance of Volmar and also traveled, preached, and corresponded with popes, emperors and kings. She transcribed her own music, whose beauty, mystical qualities, and unexpected use of wide intervals has been compared to a Gothic cathedral. Hildegard's conception of music, that it was a means for rising up to God, was analogous to that of Sufism, a tradition remote from her experience. Hildegard is considered the mother of music therapy because she praised the curative properties of music. Her death at the age of 81 years came after a long life that did not lack conflicts with authority, in which she prevailed because she was both shrewd and greatly respected. She nonetheless always declared herself a “poor, weak creature” and humble servant of God. Official recognition came only much later, when Pope Benedict XVI named her a Doctor of the Church in 2012.
Historical Context and the Basis for Hildegard's Medical PracticesHildegard fit perfectly into her times, the 12th-century renaissance when remarkable social, economic, and political changes were taking place. In many ways this period foreshadowed both the 15th-century Renaissance and the scientific advances that began to emerge in the 17th century. In spite of a rudimentary education—as evidenced by her frequent mistakes when writing in Latin—it is reasonable to infer that she had access to books like the Physiologus, a collection compiled by an unknown hand that brought together the teachings of Pliny, Aristotle, and Plutarch as well as descriptions of minerals, plants, and fantastical animals, along with many allegories.
Hildegard made use of curative techniques like cautery, scarification or bleeding that were typical of her time, but she also introduced modifications and new procedures. Her thoughts on the humors stemmed from the classical Greek theory of disease, but her notions of them suggested influences from the Orient. She conceptualized disease as something that was “lived” rather than “imposed.” Thus, she understood that pain could be perceived differently according to the patient's internal state and that those who successfully strived to be at peace would suffer less. However—and without setting aside her mysticism—she based her pathophysiological interpretations on empirical observation, conceiving the human body to be a machine that responded to physical forces that could be explained with science and reason. She made advances toward a microbiological theory of disease, which would be articulated for the first time only much later by Fracastoro in the 16th century. Even though she lacked an adequate vocabulary to describe her notion of certain pathogens, she wrote of them as the visible animals she called vermis or pediculus and smaller ones she called vermiculi. Others that could not be seen by the naked eye she called gracilimi or minutissimi vermiculi. Her work reveals her to be an open, independent thinker and fair-minded as well, unfettered by medieval authorities, whose notion that the classical authors were practically infallible held free thinking in check.6 Her view of female sexuality (see Appendix), in which relations between men and women were between equals who complemented each other, was absolutely revolutionary for her time.
Hildegard's 2 books, which were initially combined in a single volume titled Liber subtilitatum diversarum naturarum creaturarum, discuss physiology and medicine, addressing different readerships. Physica1 is theoretical, seeks a general reader, and describes the qualities of plants, land and sea animals, and minerals. Diseases are only mentioned in the section devoted to cereals and other plants. Causae et curae,7 on the other hand, is eminently practical, offering systematic descriptions of bodily functions and diseases along with the means to cure them. The present paper focuses on the dermatologic diseases and treatments the Sybil of the Rhine described in these 2 books. Included are the properties of plants, trees, and cereals that could be used to treat them.
Skin Diseases and TreatmentsOne of the main problems in the interpretation of historical texts about diseases is determining whether the name given to a condition in the past corresponds precisely to a condition called by the same name in modern medicine. We can be fairly confident, for example, that the disease referred to as scrofula in medieval texts is truly the one we call scrofuloderma today, given the characteristic clinical sign of ulcerative cervical lymphadenitis. Erysipelas generally corresponded to an acute, life-threatening inflammatory process with systemic symptoms, one that was confused with ergotism in the 12th century.8 However, we cannot be so confident about the nature of the disease Hildegard referred to as leprosy, which might have been any scaling or ulcerative skin disease involving erythema or might also have been psoriasis.9 Or references to scabies in these texts might actually have been cases of eczema of diverse types or some other pruritic skin condition. That said, we will enumerate some of the diseases Hildegard discussed and describe the ideas she held about them and her approaches to treatment.
AlopeciaHildegard sensed there was a difference between facial and scalp hair, stating in Physica1 that “it often happens that people whose scalps are largely bald have a heavy beard, while those who have a thin beard have abundant hair on their heads.” It is interesting that this astute woman concluded that hair is not of the same type in all locations. Today we know that differing sensitivity to androgens is responsible. To treat baldness, Hildegard proposed applications resembling to folk remedies: ashes of burnt plum tree bark and leaves or a mixture of bear grease and wheat chaff.
ErysipelasFor erysipelas, Hildegard prescribed magical remedies such as placing crushed flies in a circle around the lesion or rubbing the lesion with slugs or the nectar of lily or thistle. Purulent lesions should be drained by piercing them with a sliver of wood or a thorn, she claimed, but never with a cold object like a needle, nor a hot one like a red-hot iron. Success depended on the patient's avoidance of wine, heavy or fatty meals, and very hot foods. She prescribed a broth of spelt.
LeprosyLike others of her time, Hildegard distinguished between so-called white and red forms of leprosy. The first could have been a reference to the hypochromic lesions of indeterminate leprosy, or more likely it was vitiligo. The second, which was associated with a strong libido, she described as involving “broad lesional areas resembling the bark of a tree, under which the flesh is red.” This description suggests psoriasis. The treatment Hildegard favored was topical application of the bile of a hare, lily (Lilium candidum), oregano, or the droppings of swallows mixed with saffron and oil. Another more elaborate treatment included the following instructions: “take agrimony and add a third part of hyssop and twice as much asarum as of the other two, heat them together in a cauldron, and prepare a bath from these and mix in menstrual blood, as much as can be obtained.”7 Another passage explains that irascible men “who have a thick layer of flesh” should be treated by causing their skin to swell and then cutting it “to confound flesh and skin” and allow cracks to open in the skin of the nose.7 Even though these instructions were given for leprosy, they seem to be more appropriate for rosacea or psoriasis in an obese man. The nun also discussed a type of leprosy that arose from gluttony and caused “inflammations and red secretions” and yet another “that comes from the liver… and causes cuts and blackened skin and penetrates as deep as the bones.”7
PsoriasisAlthough Hildegard never referred to psoriasis per se, many passages in her work seem to describe this disease. She sometimes used the terms for leprosy or scabies as well as the German word Schuppenflechte, which refers to a scaling disease (Schuppen= flakes or dandruff and Flechte= lichen). Mentioned are remedies based on certain plants, especially burdock, oats, wormwood (Artemisia species) or acanthus, which are very well established in Europe, and there is a Hildegardian formula for an essential oil of violet that is used fairly often in Germany even today. It is interesting to find that substances derived from these plants have been associated with the inhibition of cyclooxygenase, the nuclear factor NF-κß, and other inflammatory mediators implicated in psoriasis.10 Another surprise in Hildegard's work is to find psoriatic disease mentioned in the context of Gicht or Gigiht, a word used for gout in Middle High German but whose features could fit psoriatic arthritis.
UlcersMedieval medicine considered ulcers to arise from abscesses. It was thought best to begin by draining an abcess and then applying topical preparations. Hildegard proposed the use of deadly nightshade (Atropa belladona) (Fig. 3a). Plants of the Solanaceae family, which are rich in atropine and scopolamine, should be used in very small amounts, she wrote, because “if they are much used, they can eat the flesh and perforate it.”1 Although modern medicine does not use derivatives of this plant to treat ulcerative processes topically, we found a recent publication reporting its ability to accelerate wound healing in rats.11 The authors reported observing positive anti-inflammatory, proangiogenic, and collagen remodeling effects. Were these observations mere chance or spurious findings? As on other occasions, the nun from Bingen has managed to surprise us.
ScabiesDiagnoses given as scabies in medieval sources may refer to the disease we know by this name or to other pruritic skin diseases. Hildegard was correct, however, when she stated the disease developed “between the outer layer of the skin and underlying tissues.”12 She occasionally mentioned scabies of the nail or the scalp, which suggests to us that she may have been observing psoriasis in these locations. However, we can surmise that she intuited the parasitic nature of scabies as well as the transmission of the infestation through “lust”—sexual contact—because she wrote that it was caused by “small animals” (in Germen, Suren; in Latin, gracilimi vermiculi) and because she introduced applications of metals (sulfur and mercury) to kill the parasites along with preparations of Sisymbrium species, fern (Polypodium species), and chervil (Anthriscus silvestris) (Fig. 3b). Chervil has recently been studied for antioxidant properties (free-radical scavenging and prevention of lipoperoxidation).13 Other passages in Hildegard's writing mentioned the use of aromatic plants such as ginger or basil.
That some microorganism was thought to cause scabies is suggested by other medieval texts, such as Alfonso X's Cantigas of Holy Mary,14 but confirmation would have to wait until the 19th century, when a student of Alibert, Simon François Renucci, demonstrated that the mite Sarcoptes scabiei was the culprit. As on so many occasions, Hildegard seems to have been well ahead of her time in the surprising knowledge she possessed.
ScrofulaScrofuloderma was a common cutaneous tuberculosis in the High Middle Ages and it was thought that kings had the power to cure it by the laying on of hands (the royal touch), a practice that was carried out as late as the 19th century.8 Hildegard proposed treating it with a poultice made of vinegar, catnip (Nepeta cataria), various types of lettuce (Lactuca agrestis), and honey. Here is how she described its preparation7: “Cut the lettuce at the base according to the length of the scrofulous lesion and discard the rest, then spread lines of honey on the leaves and place them on the lesion for 3 days and nights.”
Tinea CapitisHildegard's description of tinea capitis included the interesting mention of “rodent worms” that destroy the hair, and in fact we must remember that tinea means worm.15 To cure this affliction, she recommended a preparation of the roots and stalks of peony (Paeonia rockii) (Fig. 3c) for topical application as a shampoo to remove the worms causing the disease. She also advised washing the patient's clothing with the same preparation. The peony is used in traditional Chinese medicine and is mentioned in the treatises of Dioscorides (40–90 CE). Moreover, the god of medicine, known as Asclepius to the Romans, was called Paeon by the Greeks. Modern literature surprisingly offers studies of the antifungal properties of paeoniflorin, one of the plant's components.16
Curative Plants and Grains Mentioned in the Work of Hildegard of BingenMonastic or other gardens associated with the Benedictine Rule provided monks or nuns with a place to work and meditate. They are generally subdivided into orchards (viridario), a vegetable garden, and an ornamental garden. Given Hildegard's vast botanical knowledge (Fig. 4), she must have had a large convent garden at her disposal along with documents describing the natural history of her region. We list some of the plant species available to her and their use for treating skin diseases. Described are remedies that were common in her own region as well as others from distant medical traditions. Many of these treatments have been used or are likely to be considered as novel treatments in modern scientific medicine.
Yarrow (Fig. 3d), a medicinal plant used to treat wounds, is associated with carpenters in Galicia,17,18 quite probably because they applied it often to treat workplace-related injuries. Hildegard used it to treat wounds and prevent gangrene. She directed the caregiver to wash the wound with wine and cover it with a poultice of the plant wrapped in a cloth. A millefolium has recently been studied as a treatment for injuries caused by radiotherapy, such as chemotherapy-associated mucositis, as a stimulus of fibroblasts and as an immunomodulator.19–22
Calendula officinalisHildegard treated both humans and animals with calendula. She recommended treating psoriasis—or what she called scabies—of the scalp by preparing an ointment with pork fat and calendula. This preparation was applied to the scalp to remove crusts.
Chelidonium majusGreater celandine is mentioned in all the phytopharmacopoeias of folk medicine.18 Rich in latex, this plant has vesicant and antimitotic effects and is used to cauterize calluses and warts. It also contains nicotinic acid, chelidonic acid, and several alkaloids, making it a potential narcotic, abortive, and sedating agent. Hildegard used it mainly to remove warts and other skin growths. Dioscorides, who served as a surgeon in Nero's legions, mentioned that swallows expel the juice of this plant over the eyes of their newly hatched young to open the membrane that covers them in the first days of life. Hence, the association between celandine and swallows (chelidon).
Silybum marianumCommon thistle—also known as Marian thistle—contains the familiar compound silymarin, which is used to treat hepatic lesions. It is also useful as an antidote for acute mushroom poisoning. Another compound present, silibinin, may explain the use of thistle for its antioxidant and antiaging effects. The possibility that this compound may provide protection against skin carcinogenesis by UV-B radiation was studied recently.23
Tanacetum vulgareTansy has been used to treat worms, gout, and other rheumatic conditions. Tansy cakes were eaten during Lent in medieval England to prevent intestinal worms, following the belief that this infestation was caused by eating too much fish.24
Hordeum vulgareThe uses Hildegard proposed for barley remind us of another cereal, oats, which is used in many creams and soaps even today. When these hygroscopic cereals are applied to the corneal layer of the epidermis they attract and hold water and serve to hydrate the skin. Hildegard wrote that “one whose facial skin has been made rough and coarse by the wind should cook barley in water and apply it to the face with a cloth when it is lukewarm. The skin will become smooth and soft and have a lovely color.”7 As we can see, the Sybil of the Rhine was not averse to cosmetics.
ConclusionsThe Middle Ages have erroneously been described as dark and associated with a period of regression in human history. In fact this period was characterized by enormous creativity in technology, art, and philosophy and has been unfairly eclipsed by the Renaissance of the 15th century. Although Hildegard's life and world centered on spiritual matters, she was also a scientist and an early practitioner of empiricism thanks to her careful observation of nature. She was audacious and intelligent enough to write down her ideas for others, confronting authority at a time when heterodoxy might well lead to accusations of heresy. She described many diseases accurately and intuited their etiology. Although many of the remedies she proposed cannot be called useful from a modern perspective, her comprehensive approach to health was admirable, a direct reproach to the mechanistic, protocol-driven practice of our contemporary medicine, which leaves so little leeway to treat patients holistically.
“When a woman comes together with a man, a sense of heat in her brain, where pleasure resides, prefigures the taste of pleasure at their coupling and of the discharge of the man's seed. And when the seed has fallen into its place, that strong sense of heat from the brain we spoke of before draws the seed closer to itself and holds it, and then the woman's kidneys contract, and all her parts, which were preparing to open at the time of menstruation, now immediately close, just as a strong man encloses something in his fist. After her menstrual blood mixes with his seed, this makes them flesh and blood.” (This English translation of Hildegard of Bingen's description, like the other excerpts quoted in this article, are from the Spanish excerpts in the original-language version of this article. The authors’ note that their texts came from www.hildegardiana.es).
The authors declare that they have no conflicts of interest.
Please cite this article as: Romaní J, Romaní M. Causas y curas de las dermatosis en la obra de Hildegarda de Bingen. Actas Dermosifiliogr. 2017;108:538–543.