Leukonychia, also known as white nails, is a form of nail discoloration that has been known since antiquity. Baran et al.1 classified this rare entity in three main types: true leukonychia, when the alteration of the nail plate is caused by changes in the nail matrix; apparent leukonychia, caused by a disturbance of the nail bed; and pseudoleukonychia, in which the alteration of the nail plate is caused by an external factor such as onychomycosis. The condition is classified as totalis, partialis, striata, or punctata depending on the how the nail plate is affected.
We report the case of a 58-year-old man with human immunodeficiency virus (HIV) infection since 1992 but with no other relevant past history. Since starting antiretroviral therapy in 1993, the patient had followed several different treatment regimens using various drugs—zidovudine, didanosine, stavudine, lamivudine, and others—alternating with periods during which his medication was temporarily suspended. The patient remained clinically and immunologically stable and tolerated the drugs well until November 2009, at which time his viral load rose to a detectable level; ongoing treatment with nevirapine was maintained and lamivudine and abacavir were added to the regimen. At the time of writing, the patient continued on this treatment regimen.
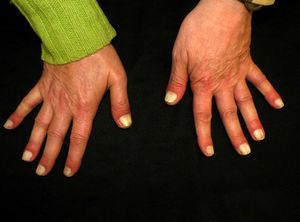
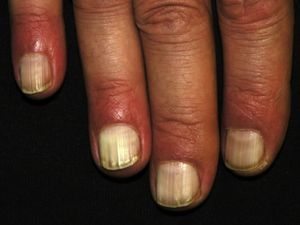
The patient was referred to our dermatology unit for assessment of whitening of the nails affecting the whole nail plate of all 10 fingers (Fig. 1). The patient stated that the leukonychia had first appeared when he started taking lamivudine and abacavir in November 2009. Having ruled out all known causes of true leukonychia and pseudoleukonychia, we diagnosed the patient with idiopathic acquired true leukonychia totalis that did not affect the toenails (Fig. 2).
Leukonychia is defined as a whitening of the nails. It was first described in 1919 by Mees,2 who found an association between this alteration of a skin appendage and arsenic poisoning. When nail plate involvement begins at the nail matrix, the condition is considered to be true leukonychia, which can be hereditary or acquired. Hereditary true leukonychia may occasionally be seen in the context of rare, complex syndromes such as LEOPARD syndrome, Bauer syndrome, and keratoderma hypotrichosis leukonychia syndrome.3,4 Acquired true leukonychia can be idiopathic or secondary to injury to the nail matrix, exposure to chemotherapeutic agents or other drugs, or underlying systemic diseases5 (measles, acute myocardial infarction, pellagra, or Hodgkin lymphoma). Pseudoleukonychia has been seen in cases of liver cirrhosis (Terry nails), hypoalbuminemia (Muehrcke lines), zinc deficiency, renal failure (half-and-half nails), and Kawasaki disease. The pathophysiologic mechanism of true leukonychia is not fully understood, although it is believed to be secondary to abnormal keratinization of the nail plate. The term pseudoleukonychia refers to an alteration of the nail plate caused by the action of an external agent.5
Although the literature contains numerous reports of mucocutaneous alterations associated with or specific to patients with HIV infection,6–8 very few nail disorders have been described in this context9,10; onychomycosis and tinea pedis are among the most common and can affect up to 1 in 3 HIV-positive patients.9,10 The next most common nail disorder in these patients is longitudinal melanonychia, which may or may not be associated with zidovudine treatment.6 Proximal or subtotal apparent leukonychia has been reported in more than 10% of HIV-positive patients, but acquired true leukonychia not attributable to a specific etiology is extremely rare.8
The existence of a direct causal relationship between antiretroviral therapy and the appearance of leukonychia is the subject of debate. According to the literature, the main antiretroviral drug involved in pigmentary changes in the skin and its appendages in HIV-positive patients is zidovudine.10 This drug can induce hyperpigmentation of the mucosas, skin, and nails, ranging from light blue to a dark grayish or brown color.3 None of the other drugs taken by our patient have been associated with the appearance of leukonychia.3 Lamivudine has been implicated in alopecia and paronychia; abacavir has been associated with hypersensitivity reactions, rhabdomyolysis, and toxic epidermal necrolysis; and nevirapine has been known to induce a characteristic maculopapular exanthem that appears 4 to 6 weeks after starting treatment.
We have described a case of acquired true leukonychia totalis in a patient with HIV infection. Our review of the literature has revealed no previous reports of cases in which the entire nail plate is affected, as occurred in our patient. In the present case, we ruled out all known causes of true leukonychia and pseudoleukonychia. While it is possible that this alteration of the patient's nails is idiopathic, we must consider the possibility that it is associated with his HIV infection and antiretroviral therapy, given the growing number of new antiretroviral drugs with potential side effects not yet described.
Please cite this article as: Pielasinski-Rodríguez U, et al. Leuconiquia total adquirida en paciente infectado por el virus de la inmunodeficiencia humana. Actas Dermosifiliogr. 2012;103:934–5.