Stiff skin syndrome is a sclerodermoid disease, observed more frequently in children, with involvement of the pelvic, scapular, and thigh regions. It is associated with prominent fibrosis of the skin layers without the inflammatory component of scleroderma or morphea.1 Clinically, it is manifest as areas of indurated skin, typically presenting without any alterations in coloration and occasionally with hypertrichosis, hyperpigmentation, subcutaneous nodules on the hands, lordosis on bending at the hip or knees, or prominent abdomen.1
Diagnosis and monitoring of this syndrome represents a clinical challenge, as induration may resemble morphea. Moreover, clinical follow-up may not indicate the true extent of involvement, and monitoring with serial biopsies in children would be invasive and not very practical.
In recent years, applications of ultrasound in dermatology have increased tremendously,2 and so far, the ultrasound pattern for Stiff skin syndrome has not been reported.
Case history. A 4year old girl, with allergy to cow milk protein and with no family history of relevance, attended the clinic due to thickening and progressive stiffness of the skin of the trunk, hips, right buttock, and left leg from when she was 2 months old. She had no limitations to joint movements.
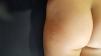
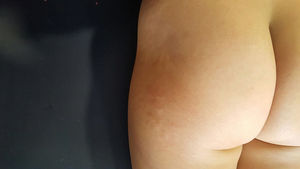
The physical examination highlighted indurated skin on the hips, lumbar region, and right buttock, with raised and irregular nodular areas without erythema, edema, local heat, or hypertrichosis. (Fig. 1).
Blood work up and C reactive protein were normal, and antinuclear antibodies, anti-DNA, and anti-ENA were negative.
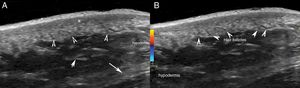
Color Doppler echotomography of the hips and right buttock was performed (Logic E9, General Electric Health Systems; Wakesha, WI; compact linear transducer of 8-18MHz), using the dermatological prototype,3 which showed focal regions of thickening and decreased dermal echogenicity, with preserved hair follicles. Nodules or defined cysts were not observed. The thickness of the dermis varied between 1.5 and 3.8mm and was greatest in the right hip. Foci of calcium deposits were not observed either inside or outside these areas. Subcutaneous adipose tissue showed a homogeneous echostructure, with unchanged thickness and prominent hyperechogenic fibrous septa. There were no signs of hypervascularization and musculotendinous planes maintained their normal morphology (Fig. 2). With these ultrasound findings, active morphea was ruled out. The findings were consistent with stiff skin syndrome.
Ultrasound. A, The grey scale (longitudinal axis; right hip) showing thickening and decreased dermal echogenicity (*) with preserved hair follicles (arrow heads). B, Color Doppler (longitudinal axis; right hip) shows absence of dermal or hypodermal hypervascularization. Note the prominent fibrous septa (arrows) in the hypodermis (A and B).
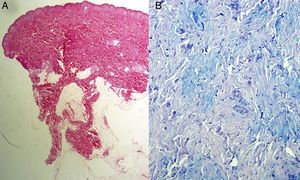
Pathology study showed a thin orthokeratotic epidermis with preservation of the dermoepidermal junction and thickening of the dermis with denser thick collagen fibers, particularly in the lower part of the reticular dermis. Thickened septa were observed in the adipose panniculus. Alcian blue staining showed increased interstitial mucin in the dermis and septa of the adipose panniculus (Fig. 3).
Considering the clinical, ultrasound, and histological findings, diagnosis of stiff skin syndrome was made.
Discussion. Stiff skin syndrome is a disorder whose pathogenesis was unknown until recently.4 The main hypotheses consider a primary anomaly of the fascia with increased production of collagen VI and congenital abnormalities of fibroblasts that lead to a noninflammatory dermis due to defective synthesis of mucopolysaccharides.5
In recent years, color Doppler ultrasound has gained increasing importance in dermatology, in view of its high definition when simultaneously visualizing cutaneous layers, underlying planes, and vascularization.6–8 To the best of our knowledge, this would be the first case in which the ultrasound morphology of this entity is described. The ultrasound signs of stiff skin syndrome are dermal thickening and reduced echogenicity, prominent fibrous septa in the hypodermis, preserved hair follicle morphology, and absence of regional hypervascularization. The most important differential diagnosis is with active morphea, in which inflammatory involvement of the dermal and epidermal layers would be observed, decreased dermal echogenicity, areas of increased subcutaneous echogenicity, and signs of dermal-hypodermal hypervascularization, with loss of hair follicle definition.9
In the future, it will be necessary to compare ultrasound images of this disease with those from other types of hamartomatous lesions, and connective tissue lesions, which are often observed in children. Perhaps some cases diagnosed clinically as hamartomas might correspond to or be associated with this entity.
Another potential use for ultrasound in this condition would be to select the biopsy site, as this method of diagnosis through imaging can delimit the regions of greatest involvement and define the depth of the lesions and their proximity to structures of risk such as large blood vessels and nerves.
In conclusion, color Doppler ultrasound can be used for the diagnosis of Stiff skin syndrome.
Please cite this article as: Kaplan V, Bolte C, Sazunic I, Wortsman X. Ultrasound Morphology of Stiff Skin Syndrome with Clinical and Histological Correlation. Actas Dermosifiliogr. 2019;110:247–248.