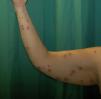
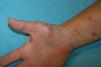
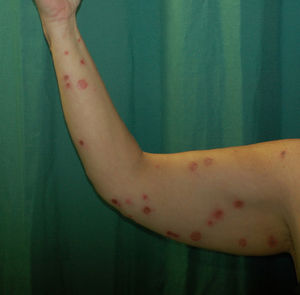
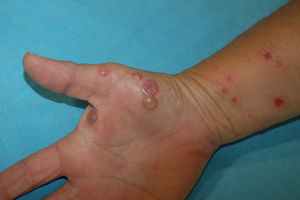
A 48-year-old woman with no past history of interest consulted for scattered pruritic skin lesions that had appeared 1 week earlier. The patient was in good general condition and had no associated systemic symptoms. Physical examination revealed nummular crusted erosive plaques of varying sizes (Fig. 1) and tense blisters, some with clear and others with purulent content, located generally on the upper limbs, the hypogastric region, and extensively on the lower limbs, covering the thighs and the pretibial region. Bullous lesions were more numerous on the right hand (Fig. 2). No mucosal lesions were observed.
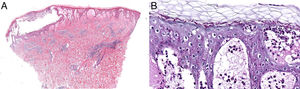
Additional TestsPurulent content from a blister was sampled for bacterial culture, and a skin biopsy of one of the lesions was performed for histology and direct immunofluorescence. Histology (Fig. 3A) showed an acute spongiotic reaction pattern, with the presence of a subcorneal blister containing neutrophils and periodic acid-Schiff (PAS)-positive filamentous structures in the stratum corneum (Fig. 3B). Both bacterial culture and direct immunofluorescence were negative.
What is your diagnosis?
DiagnosisBullous tinea.
Clinical Course and TreatmentBased on the histological findings, a complete medical history was performed, revealing previous contact with stray cats. Scales were collected for mycological culture, in which Microsporum canis was isolated. The lesions resolved after treatment with oral terbinafine (250mg/d) for 4 weeks and topical imidazole.
CommentBullous tinea, described by Costello in 1952,1 is a clinical variant of dermatophytosis, of which less than 70 cases are described in the literature. A characteristic feature is the appearance of blisters in the context of intense inflammation, usually caused by a zoophilic dermatophyte: Tricophyton mentagrophytes and M. canis are the most frequently isolated.2 The foot is the most commonly affected location. Bullous lesions are usually restricted to the edges of the plaques, and extensive lesions such as those of our patient are exceptional.3 The differential diagnosis of disseminated bullous lesions in adults is broad and includes infections, contact dermatitis, insect bites, and autoimmune blistering diseases.4 The asymmetric location of bullous lesions in tinea can help distinguish it from autoimmune blistering diseases, although differentiation is not possible in extensive cases such that described here. The secondary presentation of nonbullous tinea in the context of an autoimmune bullous disease treated with corticosteroids can also mimic bullous tinea.5 Dermatophytosis can be distinguished from bullous tinea because the former consists of a hypersensitivity reaction to a distant dermatophyte, and direct examination and culture are negative.6
Bullous tinea responds to the usual treatment regimen for dermatophytosis.6 However, due to the higher rate of terbinafine resistance of M. canis, prolonged treatment with higher than recommended doses should be considered in these cases.
The present case illustrates an unusual manifestation of a common dermatosis that should be included in the differential diagnosis of bullous lesions in the relevant epidemiological context.
Conflicts of InterestThe authors declare that they have no conflicts of interest.