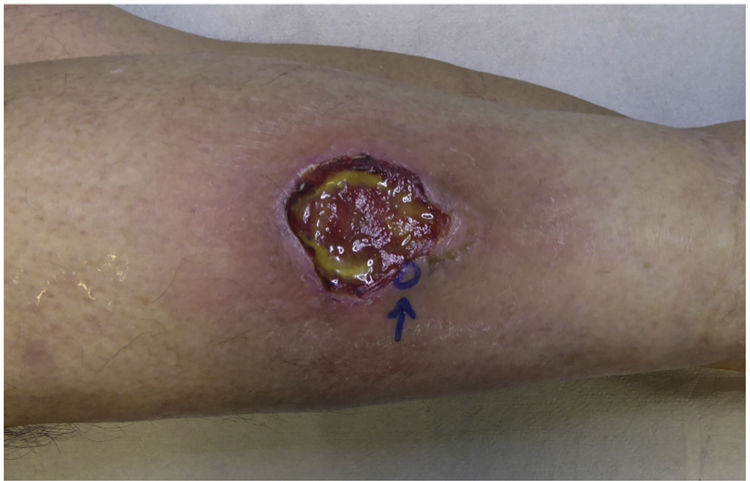
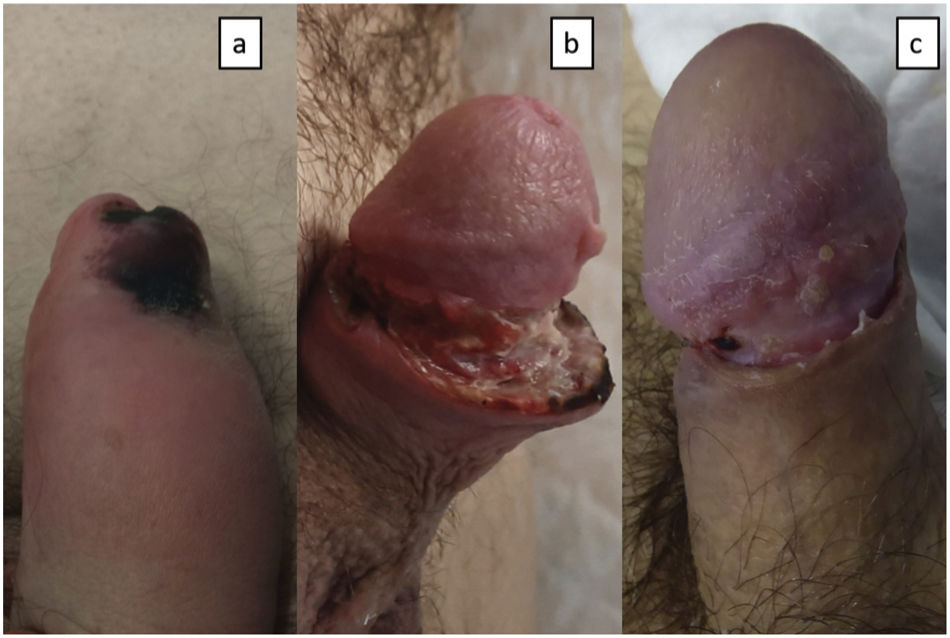
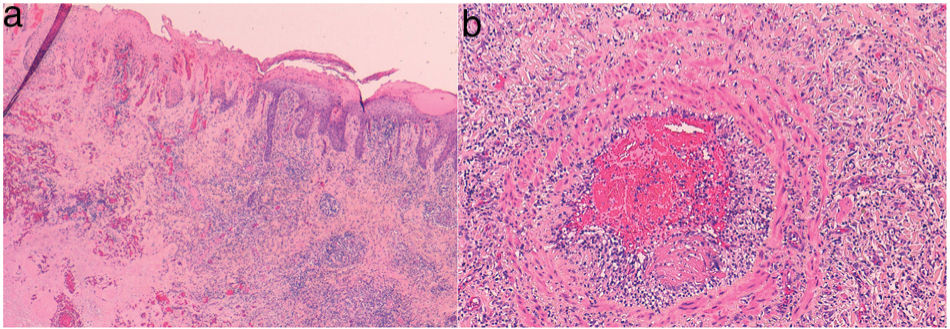
A 53-year-old man with a 15-year history of poorly controlled rheumatoid arthritis was undergoing treatment in general surgery for a 2-month-old ulcer of torpid course on his left leg developed after trauma (fig. 1). The patient was referred to the Dermatology Unit following the appearance of new ulcers in the genital area. Upon examination, a necrotic plaque was observed on the glans and foreskin with edematous penile shaft (fig. 2a). In the groin, large, soft, and movable lymphadenopathies were palpated. The empirical diagnosis of primary syphilis was followed by the intramuscular injection of 2,400,000 IU of penicillin. Additionally, a blood sample was drawn for a complete blood count including serology for HIV, hepatotropic viruses, and syphilis. In urology, a circumcision was performed to remove the necrotic eschar, adding prednisone 30mg/24h. However, the patient returned to the hospital 1 week later with suture dehiscence and increased necrosis size (fig. 2b). The serology test was negative, and the blood count showed leukopenia (1200/μL), neutropenia (150/μL), and anemia (hemoglobin 11.2g/dL). The histopathological examination of the surgical specimen revealed the presence of ulceration, chronic inflammation, vasculitis with thrombosis, and ischemic necrosis (fig. 3).
No spirochetes were identified with immunohistochemistry, nor mycobacteria with Ziehl-Neelsen, and PCR for Chlamydia trachomatis (C. trachomatis) and Neisseria gonorrhoeae in tissue tested negative.
What is your diagnosis?
DiagnosisGenital pyoderma gangrenosum.
CommentsThe patient returned for a follow-up visit with worsening of his left leg ulcer, whose biopsy also turned out to be consistent with pyoderma gangrenosum. This diagnosis was followed by the infiltration of 40mg of triamcinolone acetonide on both lesions and oral cyclosporine A (3.5mg/kg), leading to the complete resolution of the lesions within 2 months (fig. 2c). The patient remains stable on 100mg/day of oral cyclosporine and deflazacort 6mg/day. During follow-up in internal medicine, the abdominal ultrasound revealed the presence of splenomegaly. After ruling out hematological disease as responsible for the neutropenia and considering the patient's rheumatoid arthritis, he was diagnosed with Felty's syndrome. The patient is currently awaiting evaluation to start anti-TNF treatment for disease control.1
Pyoderma gangrenosum is a non-infectious neutrophilic inflammatory dermatosis clinically characterized by the appearance of erythematous nodules or pustules that progress to ulcers.2 Approximately 50% of patients have an associated systemic disease, with rheumatoid arthritis being one of the most common ones, especially in aggressive forms of the disease, as in our patient who had accompanying Felty's syndrome.3 This syndrome is a severe form of rheumatoid arthritis characterized by the simultaneous occurrence of splenomegaly and neutropenia. Pyoderma gangrenosum does not have a specific histological pattern, but a mixed dermal infiltrate along with ulceration, epidermal necrosis, and edema4 in the absence of other detectable infectious agents. Leukocytoclastic or lymphocytic vasculitis phenomena are a common finding. The treatment of choice is corticosteroids and cyclosporine A. Other therapeutic alternatives include mycophenolate mofetil, infliximab, and IV immunoglobulins.3
Lesions of pyoderma gangrenosum are often found on the lower extremities, with genital involvement being an exceptionally rare finding,5 as it can be mistaken for Fournier's gangrene. In this entity, debridement is the treatment of choice to prevent progression.6 Conversely, aggressive surgical measures to treat pyoderma, such as circumcision—as in our case—are contraindicated as they tend to worsen the lesions.
When pyoderma is found in the oral or genital region, differential diagnosis with ulcerative sexually transmitted diseases is mandatory.7 Syphilis is characterized by a single painless ulcer. Chancroid (Haemophilus ducreyi) causes painful ulcers and suppurative inguinal lymphadenopathies. Lymphogranuloma venereum (C. trachomatis) obstructs lymphatic flow, causing chronic genital tissue edema and accompanying lymphadenopathy. The diagnosis of these entities can be confirmed through specific serological tests and PCR.
The dermatologist's intervention is of paramount importance in the diagnosis of ano-genital disease, as seen in this case of atypical location pyoderma gangrenosum. A thorough patient's history and complete skin examination are essential to achieve diagnosis. Our participation is key to avoid aggressive surgical measures, which can condition the patient's progression and final prognosis.
Conflicts of interestNone declared.