Primary cutaneous CD4+ small- to medium-sized pleomorphic T-cell lymphoma is included as a provisional entity in the group of primary cutaneous peripheral T-cell lymphomas, both in the latest WHO classification of tumors of hematopoietic and lymphoid tissues and in the WHO-EORTC classification for cutaneous lymphomas.1,2 This lymphoma is defined by a predominance of CD4+ small- to medium-sized pleomorphic T cells, with no prior history of macules or plaques that would suggest mycosis fungoides.1,2
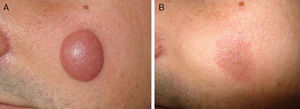
A 35-year-old man visited our department with an asymptomatic lesion on his left cheek; the lesion had appeared 4 weeks earlier and had grown rapidly. The only relevant information in the patient's past history was that he had taken allopurinol for 3 months to treat asymptomatic hyperuricemia. He had interrupted this medication 3 days before visiting our department. Physical examination revealed an oval, dome-shaped erythematous tumor measuring 3 x 4cm on the left cheek. The tumor had well-defined borders and a shiny surface and was indurated on palpation (Fig. 1A).
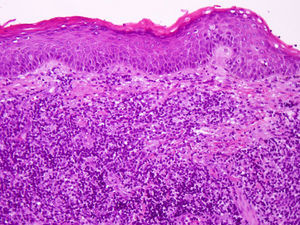
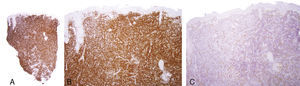
A biopsy of the lesion was taken for histopathology study. The low-magnification view showed that the epidermis was not involved and revealed a dense cellular infiltrate occupying the entire thickness of the dermis and reaching the subcutaneous tissue. The neoplastic infiltrate consisted predominantly of small- to medium-sized lymphocytes with moderate pleomorphism and mild atypia. Numerous histiocytes were also found among the lymphocytes (Fig. 2). Immunohistochemistry showed the cells to be strongly positive for CD3, CD4, and CD5. Furthermore, staining was focally positive for CD8, CD20, and CD68, but negative for CD7 and CD30. The analysis of T-cell clonality using PCR for the T-cell receptor gamma (TCRG) gene showed monoclonal rearrangement. On the basis of these data we established a diagnosis of primary cutaneous CD4+ small- to medium-sized pleomorphic T-cell lymphoma.
Further tests included an analysis of lymphocyte populations and immunoglobulin levels, computed tomography of the neck, thorax, abdomen, and pelvis, and bone-marrow biopsy. All results were normal or negative. The lesion underwent a rapid spontaneous reduction in size and was completely flat after 6 weeks of follow-up (Fig. 1B). The area of residual hyperpigmentation was not infiltrated or hard to the touch. The patient subsequently underwent local radiation therapy using a 6-MeV electron beam, with a total dose of 4000 cGy administered at a dosage of 200 cGy per day. He remained asymptomatic at 7 months (Fig. 3).
Primary cutaneous CD4+ small- to medium-sized pleomorphic T-cell lymphoma is a rare disease and accounts for just 2% of all primary cutaneous lymphomas.2 Clinical presentation is usually as a solitary plaque or tumor, typically located on the face, neck, or upper torso; it is asymptomatic and fast-growing.3–6 Spontaneous total remission of the lesions, as occurred with our patient, has been previously reported in only 1 case.3
Histology reveals dense nodular or diffuse dermal infiltrates that tend to infiltrate the subcutaneous tissue. Focal epidermotropism is a possible finding and means that a diagnosis of mycosis fungoides should always be considered.1,4,6,7 By definition, there is a predominance of CD4+ small- to medium-sized pleomorphic lymphocytes, although up to 30% of large pleomorphic lymphocytes may be found. Cases where a higher percentage of large cells is found should be classified as peripheral T-cell lymphoma, not otherwise specified. Mixed inflammatory infiltrates have also been reported, consisting of histiocytes, B cells, plasma cells, and, in some cases, CD8+ T cells and eosinophils.5,8,9 TCRG analysis shows monoclonal rearrangement in 60% to 70% of cases.
The differential diagnosis should principally include benign lymphoid proliferations (T-cell pseudolymphoma, pseudolymphomatous folliculitis, papules, nodules, and solitary lymphoid tumors) and mycosis fungoides in its unilesional and granulomatous forms.8 In our case, the rapid, self-limiting course, together with the fact that the patient had previously been treated with allopurinol, led to an initial diagnosis of T-cell pseudolymphoma. The subsequent pathology report made it possible to establish the diagnosis of primary cutaneous CD4+ small- to medium-sized pleomorphic T-cell lymphoma.
The prognosis in these lymphomas is generally very favorable, particularly in cases of solitary lesions, and 5-year survival is around 80%.2,3,5 These cases of localized disease are usually treated with surgical excision or local radiation therapy, and more aggressive treatments such as chemotherapy are not required.1–3,6,8 However, careful monitoring with regular follow-up visits is recommended.8
The usually painless course and the clinical and histologic similarity that this type of lymphoma may bear to other cutaneous lymphoid infiltrates has led some authors to suggest the term lymphocyte proliferations of uncertain significance to refer to cases, without forcing a diagnosis, where it is not possible to determine whether the process is benign or malignant.8,10
In conclusion, we present an unusual case of primary cutaneous CD4+ small- to medium-sized pleomorphic T-cell lymphoma with spontaneous remission. Because the clinical, histologic, and immunohistochemical characteristics of this type of lymphoma may coincide with those of other cutaneous lymphoid infiltrates, a careful study is required to reach a diagnosis. Dermatologists and pathologists should be aware of this entity in order to avoid unnecessary aggressive treatments.
Please cite this article as: Messeguer F, et al. Linfoma cutáneo primario de células T pleomórficas de pequeño y mediano CD4+: a propósito de un caso con resolución espontánea. Actas Dermosifiliogr.2011;102:636-8.