A 51-year-old man presented with a very painful, rapidly growing tumor in the subungual area of the first digit of the right hand. The lesion had first appeared a month earlier. The patient had sustained a crush injury to the same digit 20 years earlier.
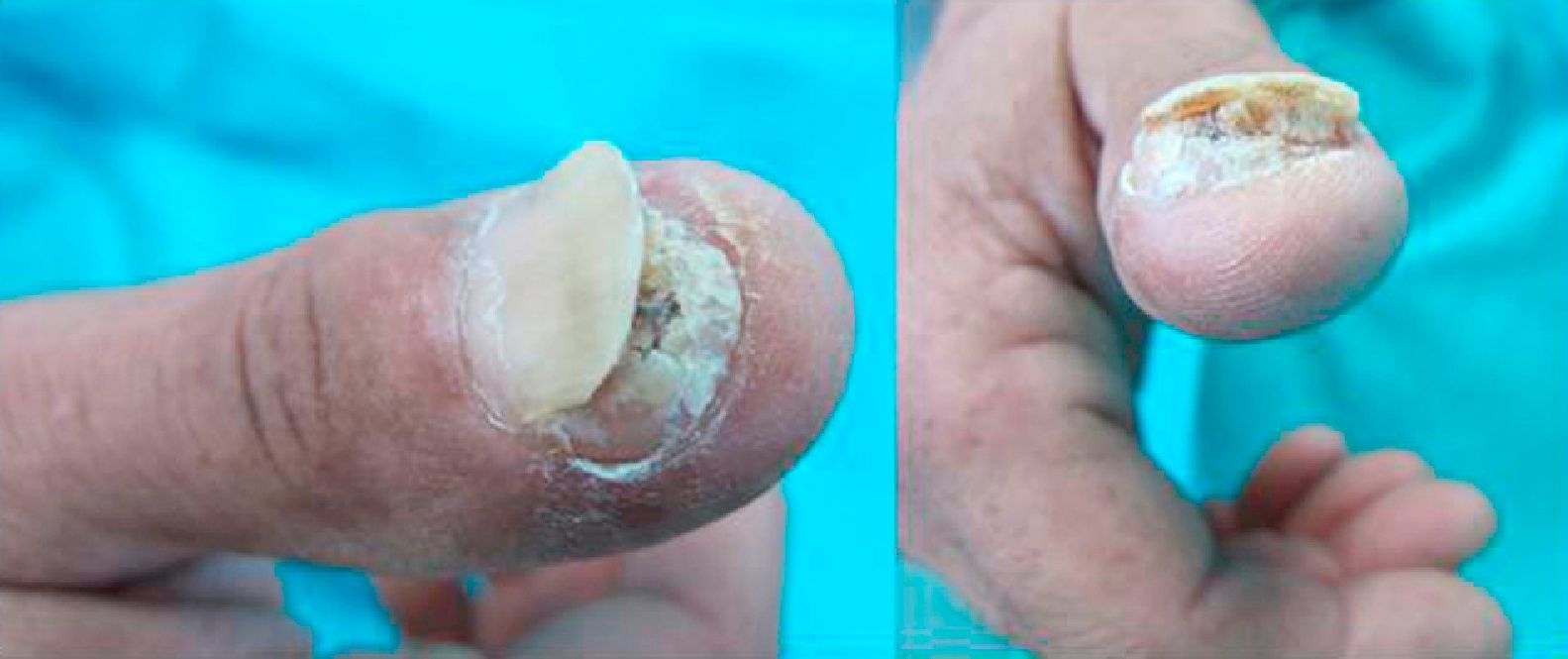
Physical ExaminationPhysical examination revealed a hyperkeratotic tumor with smooth, pink edges in the subungual area of the first digit of the right hand. The tumor was very painful on palpation and was causing the nail plate to separate from the nail bed (Fig. 1).
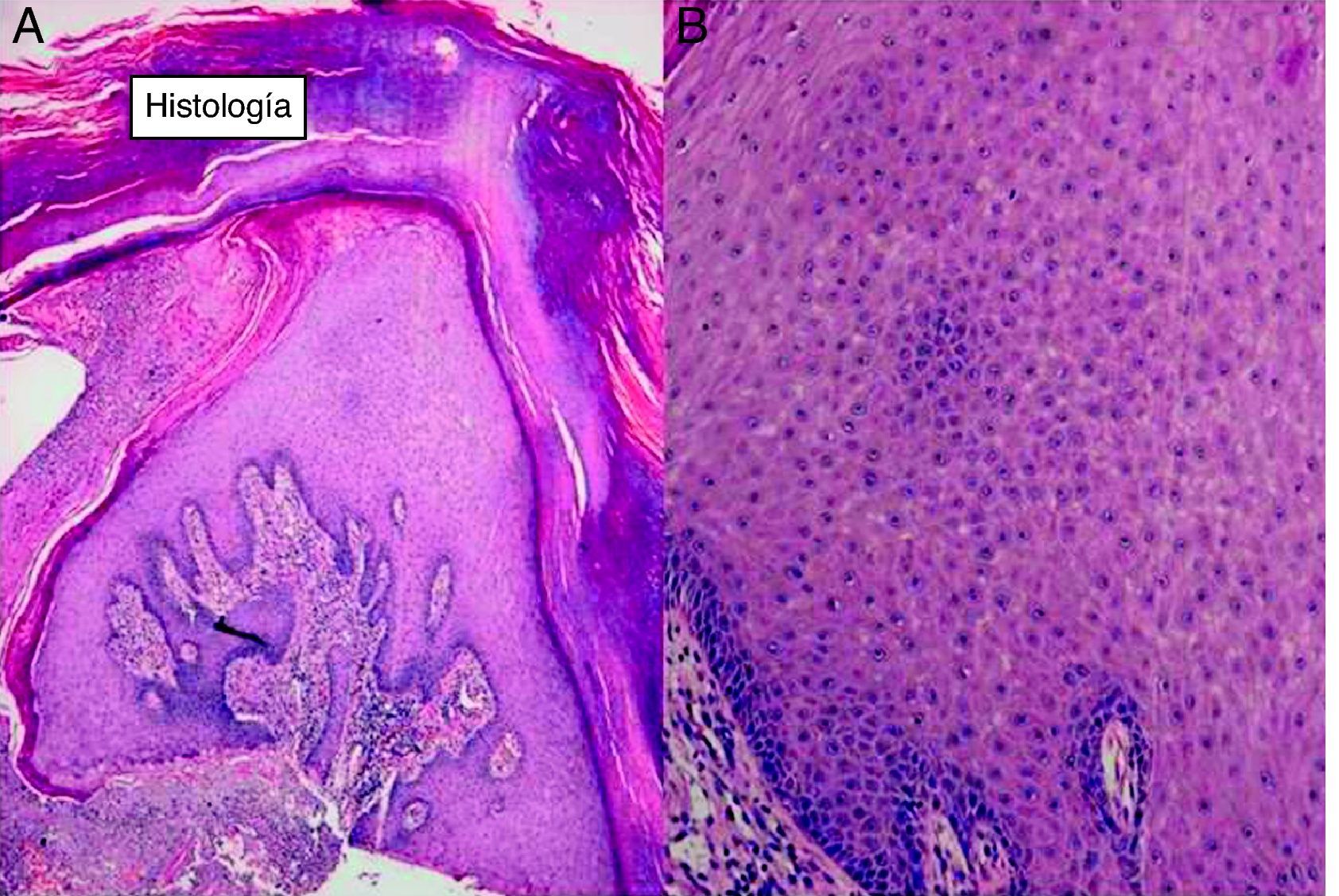
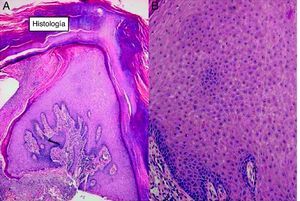
HistopathologyHistopathologic examination revealed hyperkeratosis with areas of parakeratosis, epidermal hyperplasia, and a central crater containing keratin (Fig. 2). Eosinophilic dyskeratotic cells and lymphoplasmacytic infiltrates were also observed.
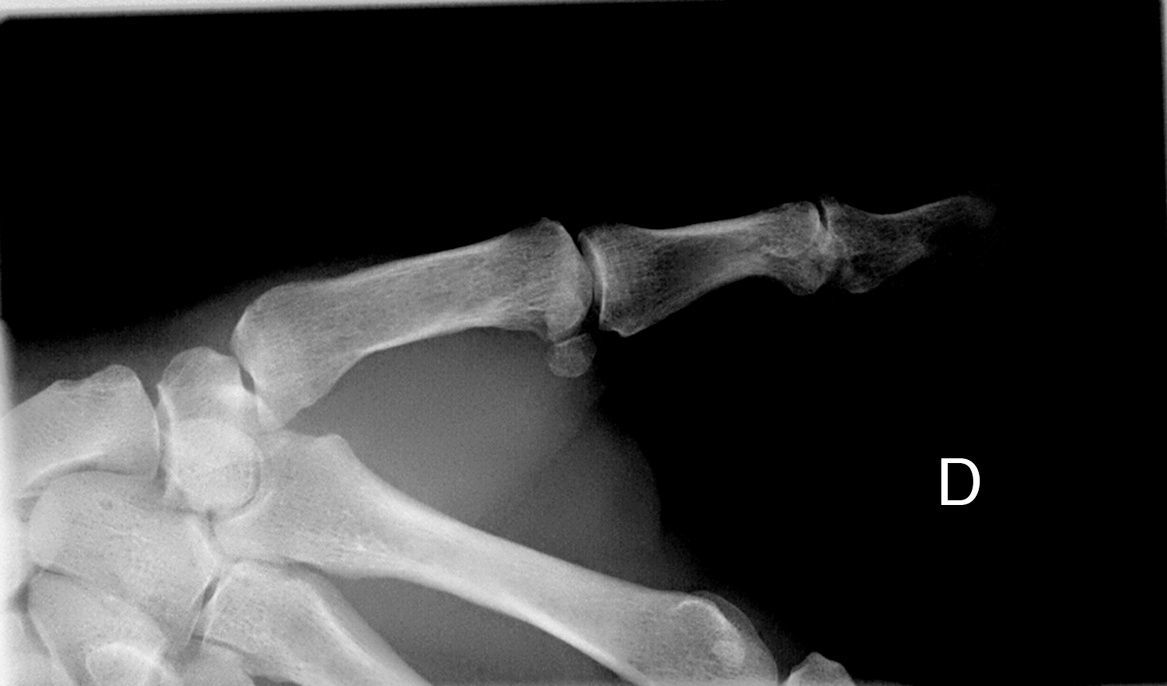
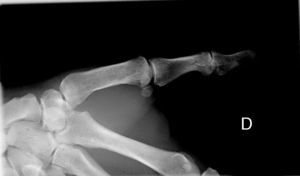
Additional TestsA plain radiograph revealed a cup-shaped lytic defect in the underlying distal phalanx (Fig. 3).
What Is Your Diagnosis?
DiagnosisSubungual keratoacanthomaClinical Course and TreatmentThe diagnosis was confirmed histologically. Because the site of the tumor affected the patient's ability to pinch with his thumb and index finger, we chose to treat him conservatively. The patient received 2 local infiltrations of methotrexate (20mg/mL) with a 1-week interval between doses. Tumor regression was achieved, allowing the residual lesion to be treated with simple curettage. After 8 months of follow-up, the patient showed no signs of local recurrence or disease progression and partial reossification of the bone defect was observed in serial radiographs.
CommentSubungual keratoacanthoma is a rare, aggressive form of keratoacanthoma that was first described by Fisher1 en 1961. Most common in middle-aged men,2 the disease presents as a painful, hyperkeratotic tumor on the distal phalanx of a finger, in most cases the thumb.2 Characteristically, the tumor grows rapidly2 and causes destruction of the underlying bone. Subungual keratoacanthoma is often preceded by a history of trauma,2 as in the case of our patient.
Unlike common keratoacanthoma, subungual keratoacanthoma affects hairless skin, lacks epithelial cords,3 tends to invade deep tissues, and rarely regresses spontaneously.4 These characteristics explain why some authors consider subungual keratoacanthoma to be a low-grade variant of squamous cell carcinoma.5
Radiographic manifestations include the cup-shaped erosion of the underlying bone without sclerosis or periosteal reaction.2 This lytic defect of the distal phalanx appears in the early stages of the disease2,5 and is more attributable to compression by the tumor than to infiltration by the tumor of adjacent structures.2,3
Diagnosis is confirmed by histologic findings that reveal epidermal hyperkeratosis, parakeratosis, and a central crater containing keratin. The presence of eosinophilic dyskeratotic cells is essential.4
The differential diagnosis should include squamous cell carcinoma,6 carcinoma cuniculatum, and common warts.2
The first-line treatment is conservative surgery,2,3 which spares underlying bone tissue. Amputation should be reserved for cases that are recurrent or have a poor prognosis.4 Other treatments with a good response rate include methotrexate, which can be administered either systemically or, as in the case of our patient, by local infiltration. The use of local 5-fluorouracil has been associated with modest improvement.7
In conclusion, we present the case of a patient with subungual keratoacanthoma to highlight the importance of suspecting this entity in patients with painful, rapidly growing, destructive subungual tumors that affect soft tissues and underlying bones. Our patient responded well to local infiltration of methotrexate. This treatment can be used as an alternative or adjuvant therapy to conservative surgery.
Please cite this article as: Perelló-Alzamora MR, et al. Tumoración dolorosa de rápido crecimiento en la región subungueal del primer dedo de la mano derecha. Actas Dermosifiliogr. 2013;104:347–8.