Lipoblastoma is a benign adipocytic tumor consisting of lobulated, immature white fat cells with a prominent capillary pattern and, frequently, a focal myxoid matrix.1 The tumor can be localized or diffuse, occurs predominantly in infancy and early childhood, and affects patients aged 5 years or younger in 84% of cases.2 Nevertheless, rare cases have been reported in adolescents and adults.3,4 Most lipoblastomas are subcutaneous lesions affecting the arms and legs, and they are more common in male patients.2
We report the case of a distinctive mesenchymal neoplasm of the lip showing adipocytic differentiation in an adult woman. We consider that this tumor is akin to infantile lipoblastoma. As far as we are aware, only 1 such lesion has been previously reported.5
A 36-year-old woman presented with a history of a small asymptomatic, pigmented, raised nodule on the vermilion border of the lower lip that had been present for about 9 months. The patient had not undergone lip piercing, filler injection for lip augmentation, or any other interventions. Her past medical history was not significant for systemic disease. Physical examination revealed a soft, brown-colored, sessile nodule measuring 0.8×0.4cm on the right half of the lower lip. The clinical diagnosis was melanocytic nevus. The lesion was completely removed.
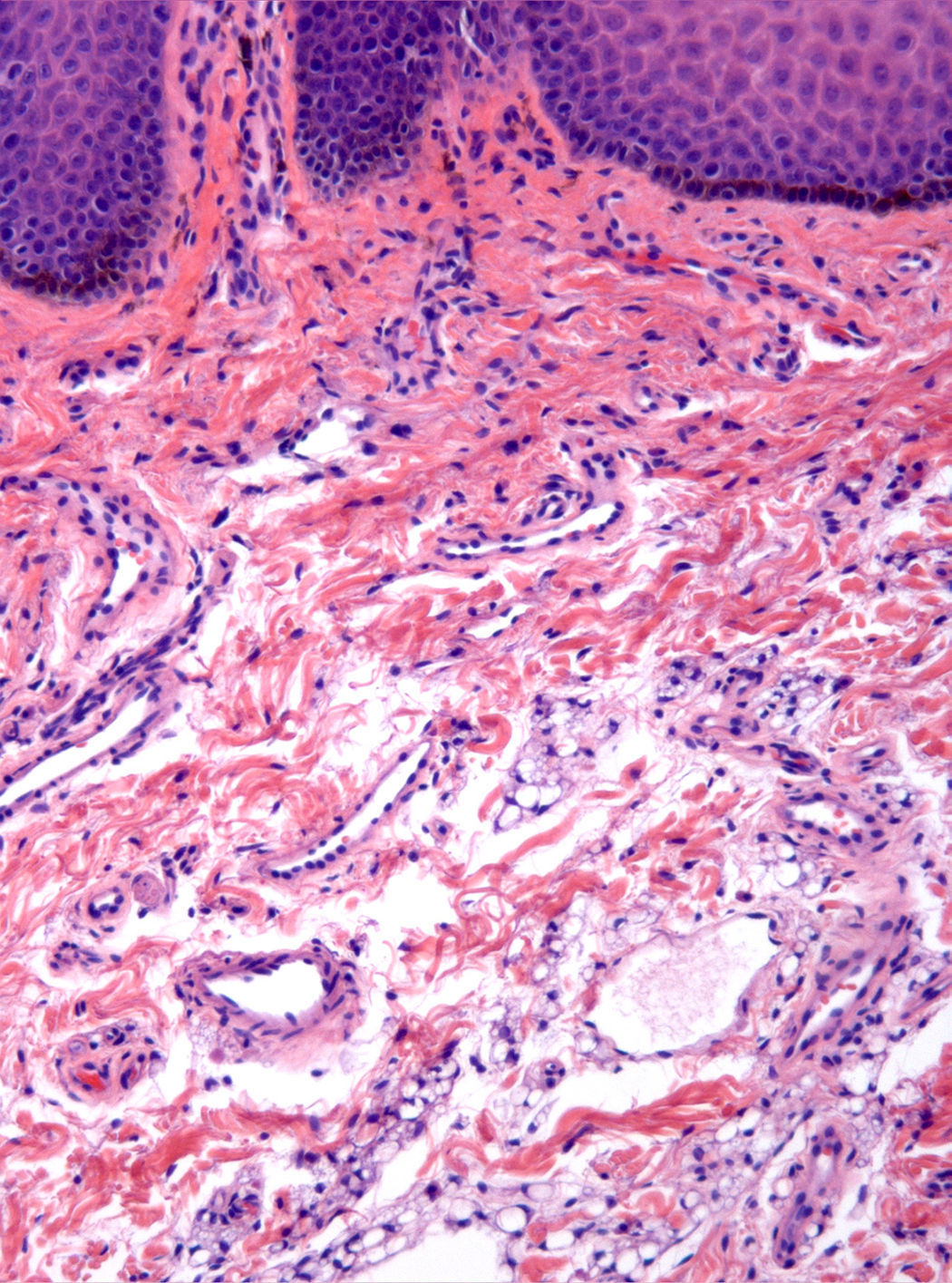
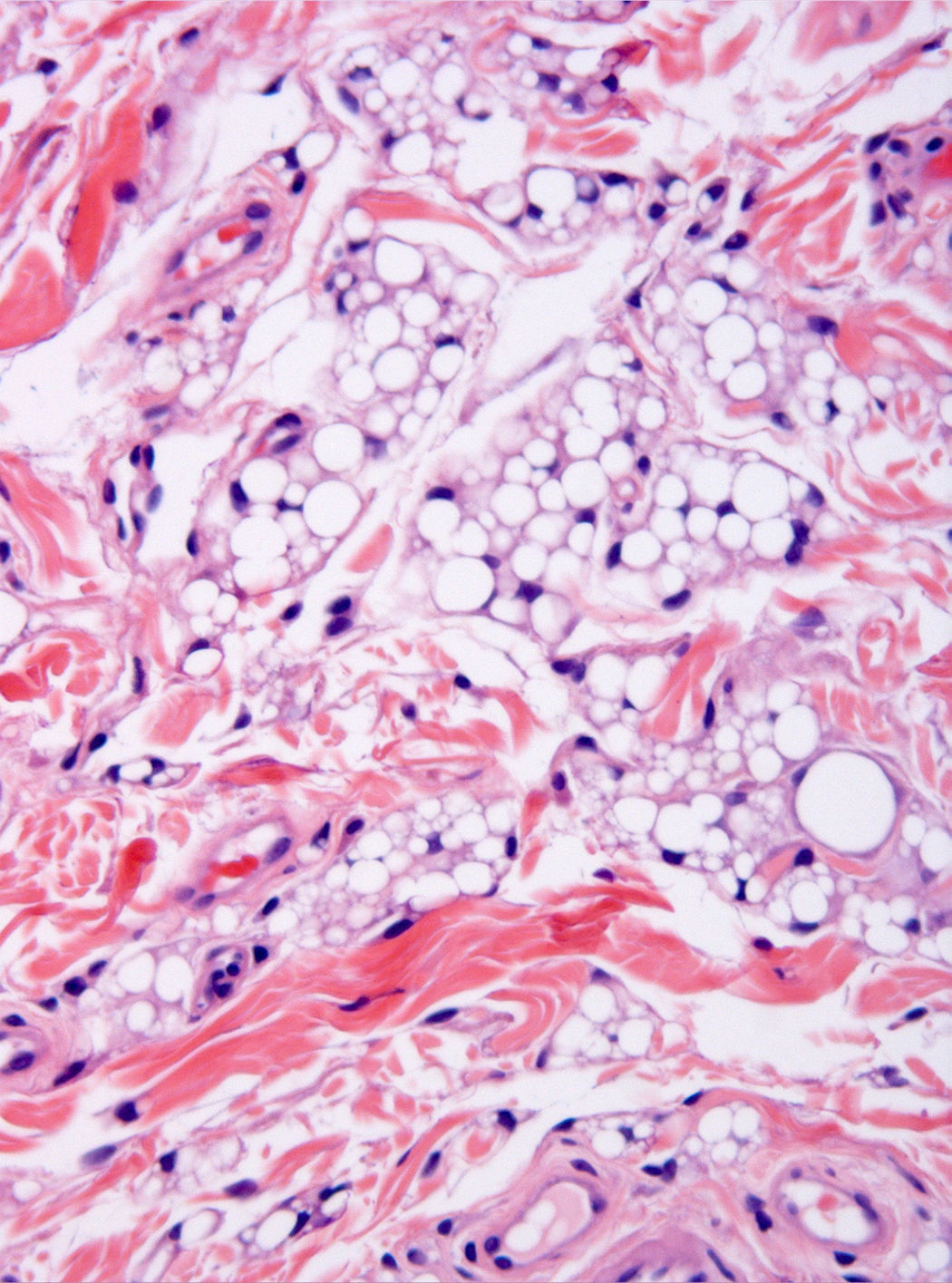
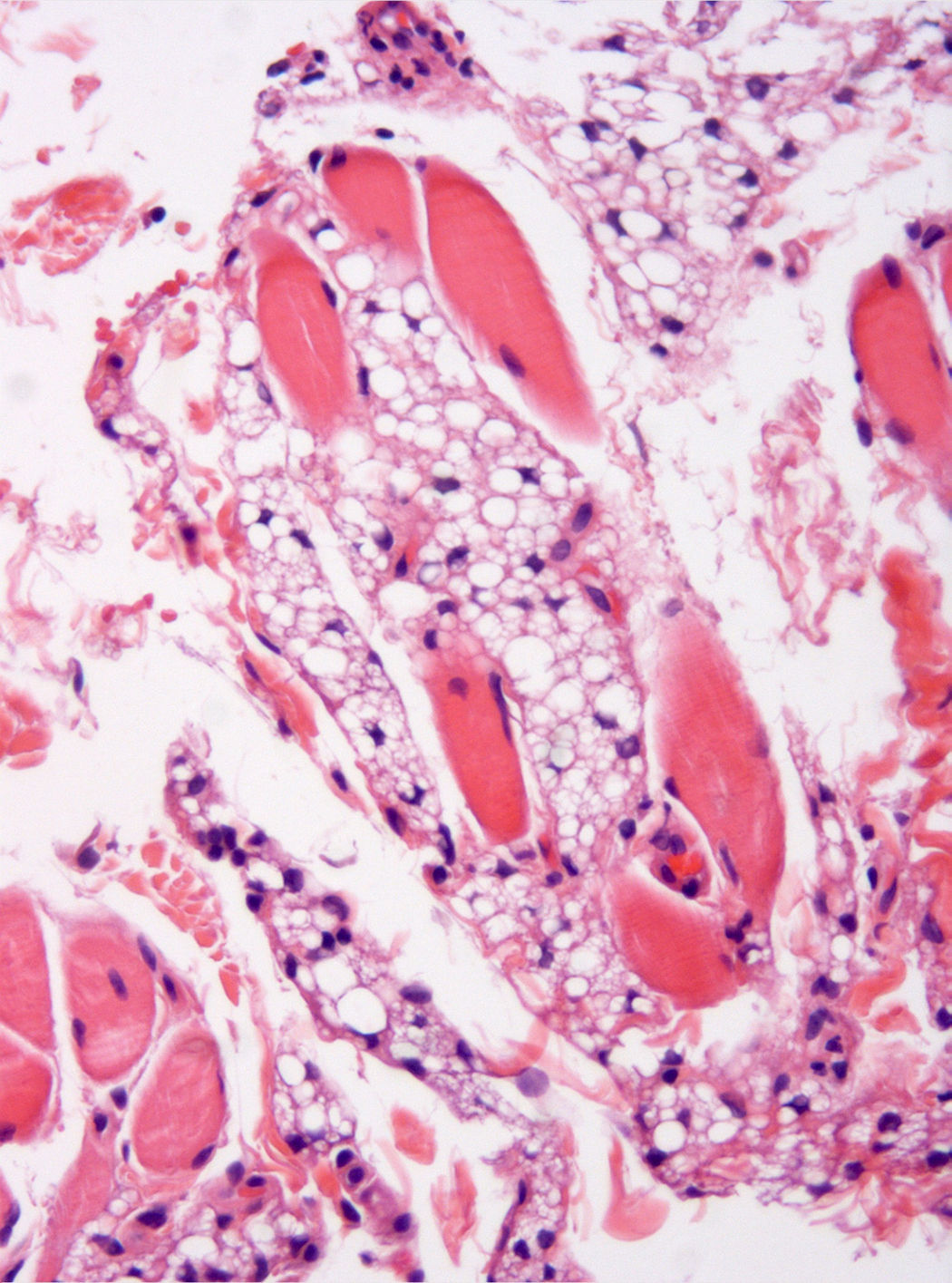
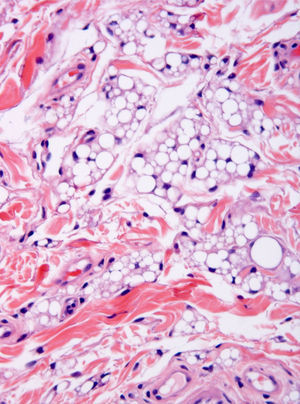
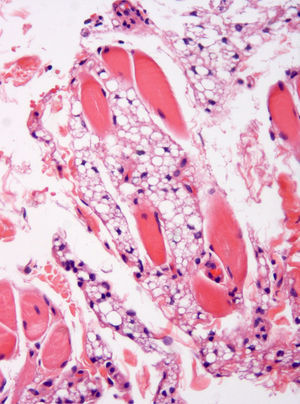
The microscopic study showed a poorly demarcated lesion, with epidermal acanthosis, irregular papillomatosis, and hyperpigmentation of the basal layer. Scattered aggregates of immature fat cells replaced much of the submucosa (Fig. 1), with a preferential perivascular location. These cells showed variation in size and were multivacuolated lipoblasts, which indented the nuclei and were interspersed with univacuolated lipoblasts that displaced the nuclei and looked like signet-ring fat cells. Mature adipocytes were scant (Fig. 2). Hibernoma-like cells were not seen. All the nuclei were small and monomorphic without atypia. Mitotic figures were absent. No giant cells, lymphocytes, mucin deposits, or plexiform vascularization were observed. Dermal aggregates were surrounded by numerous small vessels, and were incompletely separated by the thick collagenous bundles of dermis. In the depth of the lesion, lipoblast aggregates were seen to form part of the adventitia of small veins or to infiltrate between the fascicles of the orbicularis muscle (Fig. 3). No birefringence was observed in the adipocytic cells. Alcian blue (pH 2.5) did not show any acid mucin in the fat cell groups or in the dermal connective tissue. The cells stained positively for vimentin and retinoblastoma antibody and negatively for AE1/AE3 cytokeratin, CD34, CD31, CD68, and estrogen receptor. Immature adipocytes showed moderate amounts of cytoplasmic mitochondria around fat vacuoles that were visible with the antimitochondrial antibody. The amount of mitochondria was not comparable to that observed in the brown adipose tissue cells. The neoplasm involved the surgical margins.
There has been no local recurrence or metastasis in the 9 months since surgery.
The tumor in the case reported here shared histological features with lipoblastoma, namely prominent lobulation, immature fat cells consisting of multivacuolated and univacuolated lipoblasts admixed with mature fat cells, conspicuous capillaries, variably developed collagenous septae, and diffuse borders. The clinical manifestations suggested a diagnosis of melanocytic nevus due to the concomitant pigmented epidermal lesion. We interpret the epidermal lesion as a reactive hyperplasia that may accompany lesions of this kind.5
Lipoblastoma occurs primarily in infancy and early childhood, but it can be observed in adolescents and young adults.4 Lae et al.3 described 2 cases in women aged 23 and 38 years, and Silverman et al.6 reported a recurring lipoblastoma in a 48-year-old man.
To our knowledge, the present case is the second report of a lipoblastoma-like tumor of the lip. Jeong et al.5 reported a similar intradermal lesion involving the lower lip of a 61-year-old woman. The dermal tumor was erythematous, slightly elevated, and measured 2×1cm. The clinical differential diagnosis included Fordyce spot, nevus lipomatosus superficialis, and foreign body granuloma. The excised specimen showed abundant dermal lobules composed of lipoblasts and mature cells. The epidermis above the dermal tumor showed acanthosis and irregular papillomatosis, which is a change similar to that observed in the case we are reporting. Neither local recurrence nor metastasis was observed 1 year after surgery.
Lipoblastoma is a benign tumor, but it can return in 9% of cases.2 Recurrence may occur in the form of a mature lipomatous tumor. The differential diagnosis includes other dermal tumors with lipoblasts such as atypical lipomatous tumor/well-differentiated liposarcoma, spindle cell/pleomorphic lipoma, and myxoid liposarcoma.7
The nature of lipoblastoma remains to be explained. The structure of the lesion is reminiscent of the development of white adipose tissue. White embryonal/fetal fat is characterized by a very close association between adipocyte development and angiogenesis. Both small univacuolated and multivacuolated adipocytes form lobules with abundant delicate branching capillaries. It has been proposed that the white adipocyte precursor is derived from undifferentiated mesenchymal cells that reside in the mural cell compartment of the adipose vasculature.8–10
The embryonal/fetal structure of the lipoblastoma and its occurrence primarily in the very young suggests a hamartomatous lesion.