We read with great interest the excellent article by Moronta Castellano et al.1 on oral manifestations of Hansen disease. The authors report findings that are specific for the disease and those that occur independently. Consistent with data published to date, the authors confirm involvement of the palatine mucosa as the most common lesion. The findings affecting the palate were plaques or lepromas, which are histologically characterized by the presence of a dense lymphohistiocytic infiltrate with no granulomas in which Fite-Faraco and Ziehl Neelsen staining revealed mycobacteria. In this series, most patients were receiving multidrug treatment for Hansen disease at the time of the evaluation of the oral lesions. An interesting aspect not addressed in the text is the progress of these findings during specific treatment of the multibacillary forms of the disease.
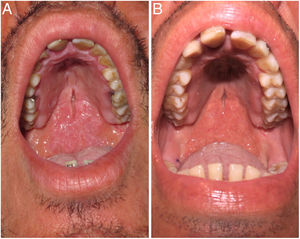
In our experience, based on imported cases, we have observed how specific oral lesions from patients with multibacillary forms of the disease responded early after initiation of multidrug treatment. The first patient was a 38-year-old man from Brazil who had been diagnosed with histoid leprosy based on clinical, histopathologic, and microbiological characteristics, with a high bacillary load in samples obtained from the skin smear and the nasal mucosa. The physical examination revealed multiple nodules and shiny plaques mainly on the face. Of particular interest on the oral mucosa, we observed a plaque affecting most of the soft palate and forming a central cleft (Fig. 1A). The patient was prescribed multidrug treatment according to the World Health Organization recommended regimen (rifampicin, clofazimine, dapsone). The first clinical check-up during the 2 subsequent weeks revealed a marked improvement in the oral lesions (Fig. 1B). The second case involved a 27-year-old woman from Brazil who had been diagnosed with lepromatous leprosy and erythema nodosum leprosum as the first manifestation of the disease. In this case, facial involvement was minimal or nonexistent, with only small lepromas on the ear lobes. A plaque similar to that in the first case was observed on the oral mucosa, again on the soft palate, although it was less thick and extensive. After initiation of multidrug therapy with rifampicin, clofazimine, dapsone, and prednisone, involvement of the palatine mucosa resolved in 10 days, with no further changes on the skin surface. Furthermore, in both patients, we observed how this improvement in the oral lesions occurred in parallel to the favorable progress of nasal symptoms (congestion, rhinorrhea). The latter observation could be explained by the fact that the oral lesions developed after extension of the bacillus from the nasal mucosa.2,3 Another aspect of interest in these patients is the presence of lesions on the oral mucosa secondary to poor oral-dental hygiene, either as a consequence of a limitation secondary to the presence of deformities (or mutilations in advanced cases) or because of a loss of motivation for self-care.3
In summary, while our observation is based on isolated cases, we wondered whether the early response of the oral lesions could act as an additional tool for monitoring adherence to multidrug therapy. Similarly, this initial response in the oral mucosa could reinforce the patient’s perception of the benefits of treatment.
Please cite this article as: Pulido Pérez A, Nieto-Benito LM, Bergón-Sendín M, Suárez-Fernández R. Réplica a «Caracterización de lesiones bucales de pacientes con enfermedad de Hansen». Actas Dermosifiliogr. 2021;112:384–385.