The cheek region can be divided into 4 areas with different cosmetic properties that must be taken into account during surgical reconstruction: buccal, infraocular or medial, zygomatic or lateral, and mandibular.1,2 Some authors have used the malar prominence, the point of convergence of the borders of these areas, as a reference point. However, the borders between these areas are not clear, depending both on intrinsic factors related to the individual's physionomy and on extrinsic factors associated with photoaging.
In large defects (>4cm diameter) affecting the medial area, the most widely used surgical reconstructions use submental or cervicofacial flaps.1,3 These types of plasty are advanced and rotated during tissue transfer. The flaps, which have a postero-inferior base, have a very rich blood supply derived from the abundant perforating vessels that arise from the transverse and facial arteries.4 Excellent results can also be achieved with island flaps, which take advantage of the abundant subcutaneous adipose tissue of the cheek; or else a combination of the 2 types of flap can be used to achieve adequate skin covering of the defect and avoid tension and secondary ectropion.5 However, the use of grafts is not recommended due to possible retraction and a poorer cosmetic result. The exception is when close monitoring is necessary to detect early recurrence.
The dissection of a cervicofacial flap must be carried out in the subcutaneous plane to preserve the subdermal vascular plexus. The plane deep to the SMAS can be used in thick defects and defects in patients with adverse risk factors for healing (smoking, radiation therapy to the area), though this carries a higher risk of neurovascular injury.2 When the tension vectors of the suture are predominantly vertical, the flap should be fixed to the periostium of the margin of the orbit and to the melonasal sulcus because of the risk of ectropion.2 Flap rotation usually gives rise to excess skin that can be eliminated using a Z-plasty or by the excision of Burow triangles, which should be designed in a way to hide scars in the base of a skin fold or crease.
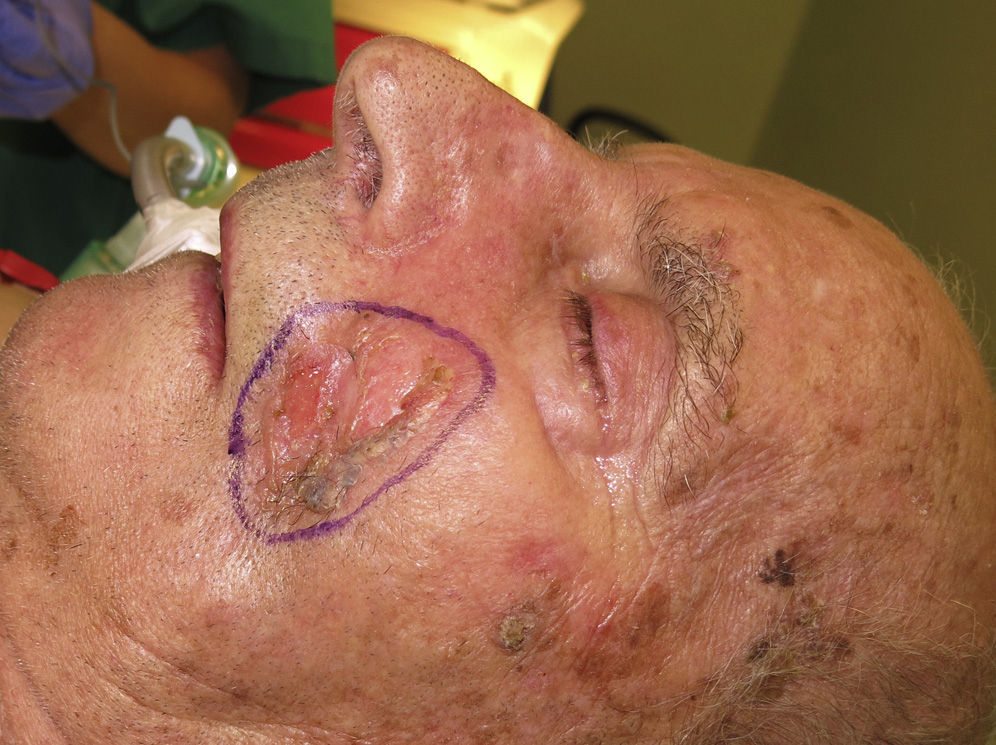
TechniqueThe patient was a 92-year-old man who was referred to our center for a rapidly growing, poorly defined, ulcerated squamous cell carcinoma of about 3cm diameter affecting the medial malar area and melolabial sulcus (Fig. 1). Given the age of patient and the rapid growth of the lesion, with bleeding and pain, it was decided to perform surgical excision.
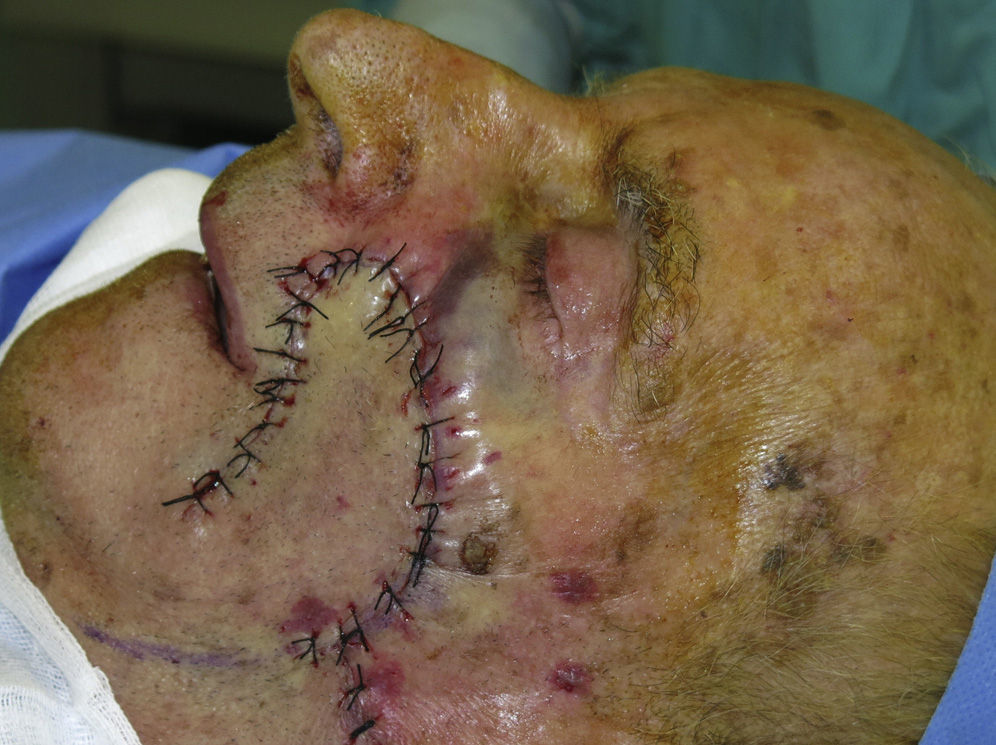
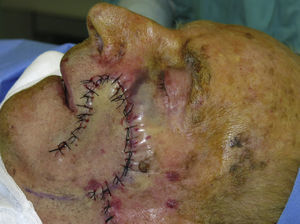
We elected to create a rotation flap (see video). Under general anesthesia, an inferior cheek flap was designed, extending the superior pole of the defect along the natural skinfold of the cheek to the cervical region. The flap was elevated in the subcutaneous plane and was rotated. After confirming good coverage of the defect, the flap was sutured with 4/0 silk. The excess skin was eliminated by 2 small tension-releasing triangles (Fig. 2).
- •
Large defects (>3-4cm diameter) of the malar subunit.
- •
Absolute: none.
- •
Relative: coagulation disorders, extrinsic factors that could predispose to cutaneous ischemia (smoking, previous radiation therapy, etc.), previous surgery to the area that could interfere with flap mobility.
- •
Surgical wound infection, including skin and deep planes.
- •
Edema, hematoma, and skin necrosis.
- •
Postsurgical ectropion.
- •
Transient or permanent alterations of sensibility and movement due to injury to nerves, vessels or muscles.
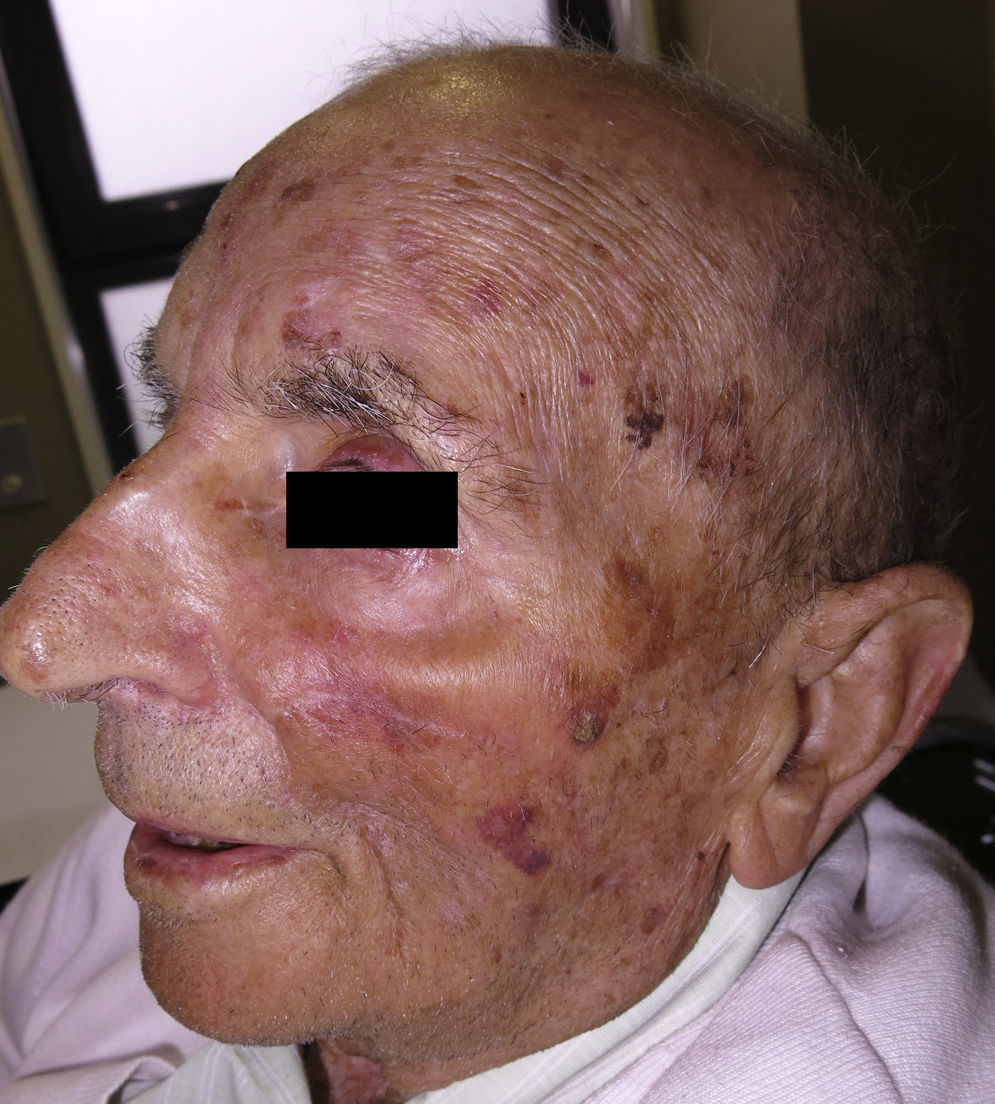
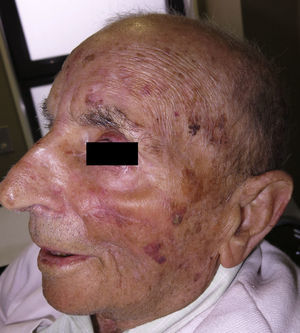
The use of a cervicofacial flap for reconstruction of the medial area of the cheek is one of the most useful techniques for the reconstruction of large surgical defects in this area.1 The operation is technically simple, though laborious if extra care is taken to minimize damage to small subjacent blood vessels to reduce postoperative bleeding; when it is necessary to mobilize skin from the cervical region, injury to the neurovascular structures of that region must be avoided.3 The cosmetic and functional results are excellent, as some of the incisions can be hidden in the facial skin folds (Fig. 3).
Conflicts of InterestThe authors declare that they have no conflicts of interest.
To José Lavigne for his help with the production and editing of the video.
Please cite this article as: Eirís N, Pérez Paredes G, Rodríguez Prieto M. Reconstrucción de carcinoma espinocelular en región malar infraorbitaria mediante colgajo de rotación-avance. Actas Dermosifiliogr. 2015;106:319–321.