Psoriasis is a chronic inflammatory disease that has been associated with cardiovascular and metabolic comorbidities, particularly in young patients and patients with more severe forms of the disease. Recent studies have also linked psoriasis to kidney disease, and this would seem only logical, as the kidney is both a target of classic cardiovascular risk factors and susceptible to the toxic effects of some of the traditional drugs used to control psoriasis.
In this article, we would like to draw readers’ attention to this recently described comorbidity and stress the importance of early detection, as once chronic kidney disease develops, it cannot be reversed. When evaluating patients with psoriasis, particularly when they are candidates for systemic therapy, we believe it is important to order laboratory tests including glomerular filtration rate and a simple urine test to screen for albuminuria (albumin/creatinine ratio).
La psoriasis es un proceso inflamatorio crónico que se ha asociado con comorbilidades cardiovasculares y metabólicas, especialmente las formas más graves y en pacientes jóvenes. Estudios recientes relacionan también la psoriasis con enfermedad renal, y parece lógico que sea así porque, por un lado, el riñón es un órgano diana de los factores de riesgo cardiovascular clásicos, y además, algunos de los tratamientos clásicos empleados para controlar la psoriasis tienen toxicidad renal. Con este artículo queremos hacer una llamada de atención sobre esta comorbilidad recientemente descrita; es fundamental su detección precoz porque una vez instaurada, la enfermedad renal crónica es irreversible. Consideramos importante que en el estudio basal de todo paciente con psoriasis, especialmente aquellos que van a recibir terapia sistémica, se analice la función renal con una analítica de sangre con filtrado glomerular y un análisis sencillo de orina para estudiar la albuminuria (relación albúmina/creatinina).
Psoriasis is a chronic and recurrent inflammatory skin disease affecting between 0.1% and 2.9% of the population worldwide,1,2 with an estimated prevalence in Spain of 2.3%.3 Disease severity is variable and the condition is not confined to the skin, but can also affect the patient's joints. In one epidemiological survey in Spain and Portugal, psoriatic arthritis was confirmed in 12.8% of patients.4 Psoriasis can also have other systemic manifestations.5 Associations have been observed between psoriasis and many other disorders, including diabetes mellitus, obesity, heart disease, hypertension, Crohn disease, cancer, and depression. In recent years, the systemic dimension of psoriasis has generated considerable interest, with a focus on prevention, early diagnosis and treatment as well as on the implications of these comorbidities on the overall management of psoriatic disease.6
Association Between Psoriasis and Systemic Disease. Cardiovascular Risk FactorsIt is possible that the association observed between psoriasis and other diseases may be due to the underlying inflammatory process that affects these patients. The most common comorbidities are obesity,7 hypertension, hyperlipidemia,8 and diabetes,9 all of which are cardiovascular (CV) risk factors. The increased CV risk in patients with psoriasis is the result of multiple factors:
- 1.
The presence of a systemic inflammatory process that gives rise to an increase in inflammatory disorders, such as atherosclerosis.10
- 2.
The higher prevalence in this population of unhealthy behaviors, including excessive alcohol consumption, smoking, and a sedentary lifestyle.11
- 3.
An increase in CV risk factors such as hypertension, diabetes, and dyslipidemia.8
- 4.
Treatment with drugs such as ciclosporin (CsA) and acitretin, which can increase CV risk. CsA can increase blood pressure and cause hyperlipidemia12 and acitretin can alter the patient's lipid profile, leading to increased triglyceride and cholesterol levels.13
Most of the evidence linking psoriasis with systemic diseases comes from observational epidemiological studies. As a result, some authors have expressed doubts about the hypothesis that psoriasis is a systemic disease and have questioned the existence of a common mechanism linking psoriasis with the observed comorbidities.11 The fact that several diseases are associated does not necessarily imply that a common mechanism exists.14 Several authors have highlighted the association between psoriasis and atherosclerosis10 and have found psoriasis to be an independent risk factor for CV disease (myocardial infarction), particularly in young patients with severe psoriasis.15 Other authors have found no such association, but those studies did not include young patients and, in most cases, the patients included did not require systemic treatment or phototherapy to control their psoriasis.16
When the mechanisms that cause the systemic and renal disorders are analyzed, the systemic inflammatory process appears to play a fundamental role. Inflammation causes an increase in insulin resistance, and levels of the cytokines present—such as adiponectin—correlate with diastolic blood pressure and low-density lipoprotein.17 The inflammation, in conjunction with the infection, provokes multiple alterations in lipid and lipoprotein metabolism, many of which are proatherogenic, increasing triglyceride and total cholesterol levels.18 Numerous studies have compared serum lipid levels in patients with psoriasis and controls. The results vary considerably from study to study owing to differences between study populations in disease severity and in the presence of comorbidities known to affect lipid metabolism, such as obesity. A general tendency has been observed towards increased serum triglyceride levels and decreased levels of high density lipoproteins in patients with psoriasis.19–21
The presence of psoriatic arthritis also increases the risk of CV disease, which suggests that the presence of a systemic inflammatory process may, by itself, be a CV risk factor.22 In severe cases, an increase has been observed in inflammatory markers, such as C-reactive protein and erythrocyte sedimentation rate.23 There have been reports of T cell activation and the production of cytokines associated with inflammation, such as tumor necrosis factor, which have been linked to an increased risk of CV events.23
Association Between Psoriasis and Kidney DiseaseThe prevalence of chronic kidney disease (CKD) in patients with psoriasis is high, with an increased risk of between 1.28 and 1.9,24 depending on the study. In this setting, kidney disease develops more often in patients with more extensive skin lesions, and severe psoriasis is an independent risk factor after adjustment for the use of nephrotoxic drugs, such as NSAIDs and immunosuppressants, and other classic factors, including age and sex.25
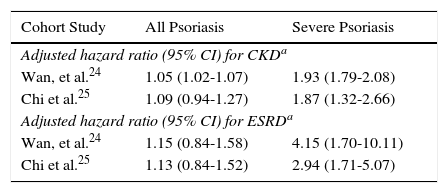
The association appears to depend on the inflammatory state characteristic of psoriasis.26 Most of the studies have found an association between psoriasis and CKD only in patients with more severe forms of psoriasis (Table 1).27 Psoriatic arthritis increases the risk of CKD and even of end-stage renal disease, for which a relative risk of 2.97 has been reported, compared with the healthy population.25
Hazard Ratio for Chronic Kidney Disease (CKD) and End Stage Renal Disease (ESRD) in Patients With Psoriasis in Two Cohort Studies.
| Cohort Study | All Psoriasis | Severe Psoriasis |
|---|---|---|
| Adjusted hazard ratio (95% CI) for CKDa | ||
| Wan, et al.24 | 1.05 (1.02-1.07) | 1.93 (1.79-2.08) |
| Chi et al.25 | 1.09 (0.94-1.27) | 1.87 (1.32-2.66) |
| Adjusted hazard ratio (95% CI) for ESRDa | ||
| Wan, et al.24 | 1.15 (0.84-1.58) | 4.15 (1.70-10.11) |
| Chi et al.25 | 1.13 (0.84-1.52) | 2.94 (1.71-5.07) |
The causes of kidney disease in patients with psoriasis are multiple. First, the kidney is a target organ for classic CV risk factors. Second, autoimmune disorders can cause glomerular impairment. Third, some of the drugs used to control psoriasis are nephrotoxic.
CKD is defined as a decrease in kidney function, represented by a glomerular filtration rate (GFR) of less than 60mL/min/1.73 m2 or as the presence of kidney injury for at least 3 months.28 Kidney injury is defined as any anatomical alteration of the organ or the presence of proteinuria or hematuria. Kidney injury can therefore be diagnosed using direct methods (histologic abnormalities on renal biopsy) or by way of markers (albuminuria or proteinuria) or abnormalities in urinary sediment or on imaging studies.
Pathological albuminuria is much more common in patients with psoriasis than in controls, and the parameters that define the severity of psoriasis correlate significantly with 24-hour albuminuria.29
The Kidney as a Target of Cardiovascular Risk Factors in PsoriasisCKD is closely related to the aging of the population and the high prevalence of diabetes and hypertension.30 Onset of kidney disease is directly related to risk factors that are highly prevalent in patients with psoriasis, such as hypertension, diabetes, obesity, dyslipidemia, and metabolic syndrome, all of which are also independent CV risk factors.31 Therefore, any of these abnormalities can develop and contribute to the progression of kidney disease.32
Since all these conditions are independent risk factors for CKD, risk is further increased by the presence of more than one of them. It is not surprising, therefore, that patients with psoriasis, who may have several of these conditions, are more likely to develop CKD. Hypertension, whether systolic or diastolic, is an independent predictor of kidney disease.33 Diabetes is also an important risk factor for vascular disease with renal involvement. Diabetic nephropathy occurs in 25% to 40% of patients with a long history of type 1 or type 2 diabetes, and is also a CV risk factor.34 Obesity and metabolic syndrome are also well known risk factors for impaired renal function.35
Psoriasis and Glomerular DiseaseMany isolated cases of associations between psoriasis and different types of glomerulonephritis have been reported, but few authors have studied this relationship in a comprehensive way. In a recent study, in which 4344 patients with psoriasis were followed up for 5 years, the authors reported an increased incidence of glomerulonephritis (HR, 1.50; 95% CI, 1.24-1.81), which may contribute to the impairment of renal function observed in this setting.26 In that study, the risk increased with severity, being higher in patients with more severe disease and those with psoriatic arthritis. The type of glomerulonephritis most frequently reported in association with psoriasis is mesangial proliferative glomerulonephritis, with and without immunoglobulin A deposits.29,36 This type of glomerulonephritis is common in infectious and autoimmune diseases and—although the pathophysiologic mechanisms are poorly understood—the increased synthesis of polymeric immunoglobulin present in such diseases would appear to be a factor in its pathogenesis.37
Association Between Drugs Used to Treat Psoriasis and Chronic Kidney DiseaseThere is lack of consensus in the literature on the relationship between CKD and psoriasis and on the role played by certain drugs used to treat psoriatic disease—CsA and methotrexate—because of the well known nephrotoxicity of both of these drugs.
The use of CsA has been linked to hypertension, kidney disease, and lymphoproliferative processes. Consequently, treatment with CsA for more than 2 years is not recommended.38 Because it causes vasoconstriction of afferent arterioles, CsA can also cause acute renal failure. Renal function improves within 5 to 7 days following cessation of treatment.39
However, prolonged treatment with CsA may cause irreversible CKD. The recommended cumulative duration of treatment and the risk associated with CsA vary from case to case, but the study that originally detected kidney damage caused by treatment with CsA concluded that patients treated for more than 12 months were at increased risk for renal impairment.40 There is evidence that the risk is not reduced by intermittent use and outcomes reported for intermittent regimens are similar to those reported for continuous treatment.41 Multiple studies in liver transplant patients have found no differences in renal function between groups receiving high and low doses of CsA and no increased association with kidney disease in patients on higher doses of the drug.42
In the case of methotrexate, 90% of the drug is eliminated through the kidneys and the damage may be caused by renal precipitation or by the direct effect of the drug on renal tubules. Methotrexate toxicity depends on the blood concentrations achieved after administration. Levels greater than 10 μM at 24 h or greater than 1 μM at 48h are associated with a high probability of nephrotoxicity, especially in older patients.43 Some studies have reported methotrexate nephrotoxicity in patients with psoriasis.44,45 Although the doses used to treat psoriasis are low and few cases have been reported, dermatologists should be aware that nephrotoxic doses may be reached because the threshold varies a great deal from patient to patient.
The use of nonsteroidal anti-inflammatory drugs has been linked to increased kidney damage in patients with moderate to severe psoriasis (relative risk, 1.69).26 In many cases, nonsteroidal anti-inflammatory agents are used in combination with methotrexate, a practice that could increase the risk of kidney damage.
The literature on biologic drugs includes multiple cases of autoimmune kidney disease caused by biologic therapy in patients with various diseases, including psoriasis.46–53 In most of these cases, the patients had membranous glomerulonephritis, although granulomatous nephritis has also been reported. These cases can be categorized as follows: glomerulonephritis associated with systemic vasculitis, glomerulonephritis in lupus-like syndromes, and isolated autoimmune renal disorders. Most of the cases reported are associated with tumor necrosis factor inhibitors.54 Notwithstanding these findings and given their lack of end-organ toxicity, biologic agents can be a good therapeutic option in patients with CKD and even end-stage renal disease. Cases have been reported of successful treatment of psoriasis with biologic drugs in patients on hemodialysis.55
Systemic Implications of Kidney Disease in Patients with PsoriasisChronic Kidney Disease as a Cardiovascular Risk FactorCKD is a major public health problem affecting 10% of the adult population and more than 20% of people over 60 years of age.56 Moreover, it is well known that the disease is underdiagnosed. CKD is an independent risk factor for CV disease, and the risk of CV mortality in patients with CKD is greater than the risk of progression to dialysis or transplant.57 CV disease associated with CKD is treatable and potentially preventable.57
It is important to be aware of the association between impaired renal function, the onset of CV disease, and death. In clinical practice, renal function should be monitored in patients in the at-risk population, who should also be routinely tested for proteinuria (albuminuria). Monitoring is essential owing to the high incidence of kidney disease in patients with psoriasis. Once a persistent elevation of albumin in the urine (microalbuminuria) is confirmed, CV risk exists even when renal function is normal. The risk increases as renal function deteriorates. In patients with end-stage renal disease, the risk of CV disease is 20 to 30 times that of the general population.58
The severity of renal impairment is assessed by measuring the GFR and by the presence of microalbuminuria (30-300 mg/24h) or macroalbuminuria (> 300 mg/24h). A GFR estimated at below 60 mL/min is defined as kidney failure and represents a significant increase in CV risk. A low GFR is often accompanied by albuminuria, and the effect of the two factors is additive. It is important to monitor and control risk factors in patients with renal impairment from the outset. Patients with renal impairment and ischemic heart disease and/or heart failure often do not receive all the treatment they should; in such cases, special attention should be paid to improving survival.59
Assessing Emerging Cardiovascular Risk FactorsIn patients with renal failure, the kidneys gradually lose the ability to excrete phosphorus. This deficit is compensated by phosphaturic mechanisms that boost the urinary excretion of phosphorus, such as increases in parathyroid hormone (PTH) and fibroblast growth factor 23 (FGF23), which maintain the normal phosphaturic capacity. The role of FGF23, a phosphatonin with 251 amino acids, is to maintain normal phosphorus levels in the body. It does this by downregulating the activity of the type II sodium/phosphate cotransporters in the proximal tubule, thereby decreasing renal tubular phosphate reabsorption. However, it also inhibits the activity of 1 alpha hydroxylase, thereby reducing synthesis of 1-25 dihydroxycholecalciferol from its precursor calcidiol, and increases 24 alpha hydroxylase, which in turn increases vitamin D catabolism. Thus, vitamin D is decreased in patients with kidney failure.60 The increases in PTH and FGF23, together with the decrease in vitamin D, increases CV risk.61
Patients with psoriasis have decreased vitamin D levels and increased PTH levels. In winter, the prevalence of vitamin D deficiency can reach as high as 80% in patients with psoriasis.62 While the origin of vitamin D deficiency in psoriasis has not been studied in depth, it may have multiple implications. First, vitamin D deficiency can cause osteoporosis, reduce the patient's immune response, or increase CV mortality and the risk of diabetes.63,64 Vitamin D deficiency also has important implications in the pathogenesis of psoriasis because certain vitamin D receptors are responsible for the growth and differentiation of keratinocytes and for the immune functions of T cells and dendritic cells.65 In fact, topical vitamin D derivatives have been used to treat psoriasis and it is also possible that an increase in endogenous vitamin D production may be one of the mechanisms of action of phototherapy in this setting.66,67 Increased serum PTH has also been observed in patients with psoriasis and this may have direct implications on CV risk in these patients.68 While it may be the result of vitamin D deficiency, increased PTH could also be a phosphaturic mechanism triggered by the decreased renal elimination of phosphorus.
Recommendations for Dermatologists on Prevention. What, When and How?Psoriasis is an inflammatory disease that often has systemic effects and is associated with several CV risk factors. It would, therefore, seem wise to take all these possibilities into account when treating these patients (Table 2).
Recommendations for Preventing Renal Damage in Patients with Psoriasis.
| 1. Assess kidney function in patients in whom 3% or more of the body surface area is affected and monitor annually in patients with moderate to severe disease. |
| Blood creatinine |
| Glomerular filtration rate calculated using formulas (MDRD-4 or CKD-EPI) |
| Urine albumin levels (moderate increases in albuminuria) |
| 2. If potentially nephrotoxic drugs are prescribed, closer monitoring of renal function is required. |
| 3. If a decrease in glomerular filtration rate or a moderate increase in albuminuria is observed, the patient should be assessed by a kidney specialist. |
| 4. Monitor classic cardiovascular risk factors: hypertension, diabetes, dyslipidemia, and excess weight or obesity. |
Abbreviations: CKD-EPI, Chronic Kidney Disease Epidemiology Collaboration; MDRD 4, Modification of Diet in Renal Disease-4.
At least in patients with moderate to severe forms of psoriasis, as in other inflammatory disorders, kidney function should be assessed at least once a year, including measurement of microalbuminuria, creatinine, and GFR (estimated using formulas). The most commonly used formulas are those taken from the Modification of Diet in Renal Disease (MDRD) study, known as MDRD-4,69 and those devised by the Chronic Kidney Disease Epidemiology Collaboration, known as CKD-EPI.70 Some authors recommend testing urine albumin levels (microalbuminuria), creatinine, and estimating GFR in any patient who has plaque psoriasis affecting more than 3% of the body surface and taking particular care if the patient is on nephrotoxic drugs, such as methotrexate or CsA, irrespective of the underlying disease.20 Even closer monitoring of renal function is needed when the patient is taking potentially nephrotoxic drugs.15 Nephrotoxic drugs are contraindicated in patients with kidney injury. Treatment with drugs such as CsA should never exceed 2 years. Prescribing treatments that are not nephrotoxic may be a reasonable alternative to reduce this risk.
When monitoring detects a decrease in GFR or a higher value for microalbuminuria compared to prior measurements, the patient should be carefully assessed, if necessary by a nephrologist. We must not forget that psoriasis is a chronic disease and that early diagnosis of renal impairment will facilitate prompt stabilization of the condition, which is important since the damage is irreversible.
Cardiovascular Risk AssessmentTo prevent CV events, it is essential to monitor the classic CV risk factors (hypertension, diabetes, dyslipidemia, and excess weight/obesity) in patients with psoriasis, especially those with moderate to severe disease. Patients with extensive psoriasis and those who have extracutaneous symptoms, such as arthritis, have a higher risk of comorbid disease.
The key messages of this study are shown in Table 3.
Psoriasis and Kidney Disease: Key Messages.
| • Psoriasis is a systemic inflammatory disease that may increase the risk of comorbid diseases, such as hypertension, dyslipidemia, and diabetes. |
| • The risk of kidney disease is increased in patients with psoriasis and particularly in patients with more severe disease. |
| • Psoriasis is associated with a higher risk of mesangial proliferative glomerulonephritis. |
| • The increased prevalence of kidney damage in psoriasis may be the result of vascular damage caused by inflammation and other comorbidities. |
| • When used for long periods, some of the drugs used to treat psoriasis are nephrotoxic. |
| • In patients with moderate to severe psoriasis or psoriatic arthritis, renal function should be monitored regularly by measuring the glomerular filtration rate. |
Abbvie organized and financed the face-to-face meetings of this working group.
Conflicts of InterestAbbvie facilitated the meetings of the workgroup, but none of the company's employees participated in the collection of scientific evidence, group discussions, or drafting the article.
Raquel Rivera has received honoria for consultancy work from Abbvie, Janssen, Lilly, and Pfizer, has served as a rapporteur for MSD, Abbvie, Janssen, Leo Pharma, Novartis and Pfizer and as a researcher for Abbvie, Pfizer, Janssen, Celgene, Lilly, Novartis, Leo Pharma, and has received funding to attend conferences from Abbvie, Janssen, Novartis, Pfizer, Leo Pharma, Celgene and MSD
Please cite this article as: González-Parra E, Daudén E, Carrascosa JM, Olveira A, Botella R, Bonanad C, et al. Enfermedad renal y psoriasis. ¿Una nueva comorbilidad? Actas Dermosifiliogr. 2016;107:823–829.