Leukonychia is whitening of the nail plate. In 1919, Mees first described leukonychia in arsenic intoxication.1 Baran classified leukonychia into true, apparent, and pseudo-leukonychia. True leukonychia can be acquired or inherited, and based on the distribution of white blotches, can be further subclassified as leukonychia punctata, leukonychia striata, leukonychia partialis, or leukonychia totalis.2 There are very few reported cases of idiopathic acquired leukonychia totalis3 and we report the present case to demonstrate this uncommon clinical entity in a 10-year-old boy and his response to micronutrient supplementation.
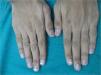
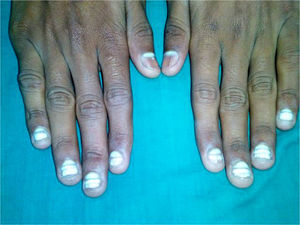
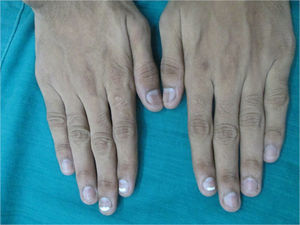
A 10-year-old boy presented at our clinic with porcelain white finger nails that he had had since 4 years of age. Leukonychia totalis and leukonychia striata were seen on the fingernails, with leukonychia partialis in both the thumbnails (Fig. 1). A detailed history demonstrated progression from leukonychia partialis to striata and totalis over the years. The strength of the nail plate was normal. Pressure over the nail plate caused no fading of the leukonychia, suggesting nail matrix origin and ruling out Muehrcke's lines (apparent leukonychia striata), a common clinical differential diagnosis.3 His hair, eyes, teeth, and the remainder of the cutaneous examination were normal. There was no clinical evidence of malnutrition, alopecia areata, psoriasis, or lichen planus. The patient gave no history of preceding illness, surgery, trauma, chemical exposure and drug intake, including herbal medicines. The patient was born out of a nonconsanguinous marriage and there was no family history of leukonychia. Repeated cultures and microscopic examination of the nail clippings with 10% potassium hydroxide were negative. All the routine investigations, including serum proteins, liver function tests, serum calcium, and zinc levels were within normal limits. With the aforementioned clinical and laboratory assessment a diagnosis of idiopathic leukonychia partialis to totalis of the fingernails was established. The patient's parents did not consent to a nail biopsy. The boy was started orally on Zinc sulfate 137.5mg (containing 50mg elemental zinc) capsule once daily, along with a single daily capsule of 8 essential amino acids and vitamins A, B complex, C, D, and E (containing 18.3mg l-leucine, 5.9mg l-isoleucine, 25mg l-lysine hydrochloride, 5mg l-phenylalanine, 4.2mg l-threonine, 6.7mg l-valine, 5mg l-tryptophan, 18.4mg dl-methionine, 2500 IU vit A, 200 IU vit D, 5mg vit B1, 3mg vit B2, 25mg vit B3, 5mg vit B5, 1.5mg vit B6, 2.5mg vit B12, 0.75mg folic acid, 40mg vit C, and 7.5 IU vit E). Two monthly follow-ups showed serial improvement at each visit, and complete resolution of the leukonychia was observed at the end of 7 months (Fig. 2). The treatment was continued for 3 months after resolution of the leukonychia, and there was no relapse in the 6 months after treatment was discontinued. The patient is presently monitored.
Leukonychia is the most common chromatic abnormality of the nail; however the physiologic mechanisms causing it are not entirely clear and Newton's theorem (i.e. a surface appears white when it reflects the radiation of visible light), has been proposed to explain leukonychia. In true leukonychia there is abnormal matrix keratinization, with persistent parakeratosis and keratohyalin granules in the nail plate, which might play a role in the modification of the light reflection by the ungual plates.3 Baran classified leukonychia into the following 3 primary types: (1) true leukonychia, where in the nail plate involvement originates in the matrix; (2) apparent leukonychia, in which the pathology lies in the subungual tissue; and (3) pseudo-leukonychia, which is due to keratin granulations, as seen in superficial white onychomycosis.2 Inherited leukonychia can be presented as an isolated condition or as one of the several other reported syndromes. There is an autosomal, dominantly inherited syndrome in which leukonychia occurs in combination with kidney stones and sebaceous cysts, with sensory-neural deafness and knuckle pads, which is known as the Bart-Pumphrey syndrome.3 Popular lay media claim that the etiology of leukonychia is due to calcium and/or zinc deficiency. However, no studies are available in the scientific literature to support or refute these claims.5 Acquired leukonychia has been reported due to trauma, drugs such as chemotherapeutic agents (e.g., anthracyclines, cyclophosphamide, vincristine, cyclosporine, fluorouracil, and methotrexate), and systemic or local infections (e.g., typhoid fever, hepatic cirrhosis, ulcerative colitis, leprosy, and recently due to selenium deficiency in Crohn's disease).3,5,6 In children, increased requirements for macro- and micronutrients during the growing years might not be met adequately through routine meals. This deficiency could not be reflected in their serum values; however it could lead to subtle manifestations of nutritional deficiencies such as leukonychia, as in the present case. Clinicians should consider oral supplementation of relevant micronutrients in cases of acquired leukonychia, even in patients for whom serum levels do not reveal any evidence of nutritional deficiency. To the best of our knowledge, only 7 cases of idiopathic acquired leukonychia totalis have been reported to date.4,7–12 Our case is the eighth addition to the list; furthermore, it is the first case of acquired leukonychia totalis of the fingernails in which a successful resolution following therapy has been reported.