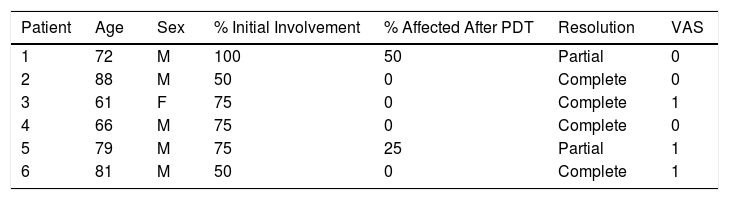
Actinic cheilitis is a chronic premalignant disease that generally affects the lower lip and that is considered equivalent to actinic keratoses of the skin.1–3 Several treatments have been proposed for actinic cheilitis, but none of these are considered definitive. Daylight photodynamic therapy (PDT) is a widely used treatment for actinic keratoses and has shown efficacy similar to that of conventional PDT, with no or minimal pain.4,5 The objective of our study was to describe the efficacy and safety of daylight PDT in the treatment of actinic cheilitis according to our experience. Between May and October 2018, 6 patients were treated. After gentle curettage, a roll of cotton wool was placed in the internal labial mucosa to expose the lower lip and sufficient quantity of methyl aminolevulinate cream was applied. Then exposure to ambient sunlight for 2 hours without occlusion was recommended. The rest of the skin was protected with factor 50+ sunscreen. After 2 hours of exposure, the treated area was washed and factor 50+ sunscreen was applied to the lip. Another session was performed 2 weeks later and the patients were examined after 2 months (Figs. 1 and 2). Patients were assessed with a clinical scale (affected area and complete/partial/no response) and a visual analogue scale (VAS) for pain. The characteristics of the study population and the outcomes of treatment are summarized in Table 1. Four of the patients (67%) showed complete response and 2 had a partial response with a mean reduction in the affected area of 58.3%. The mean score on the VAS was 0.5 out of 10.
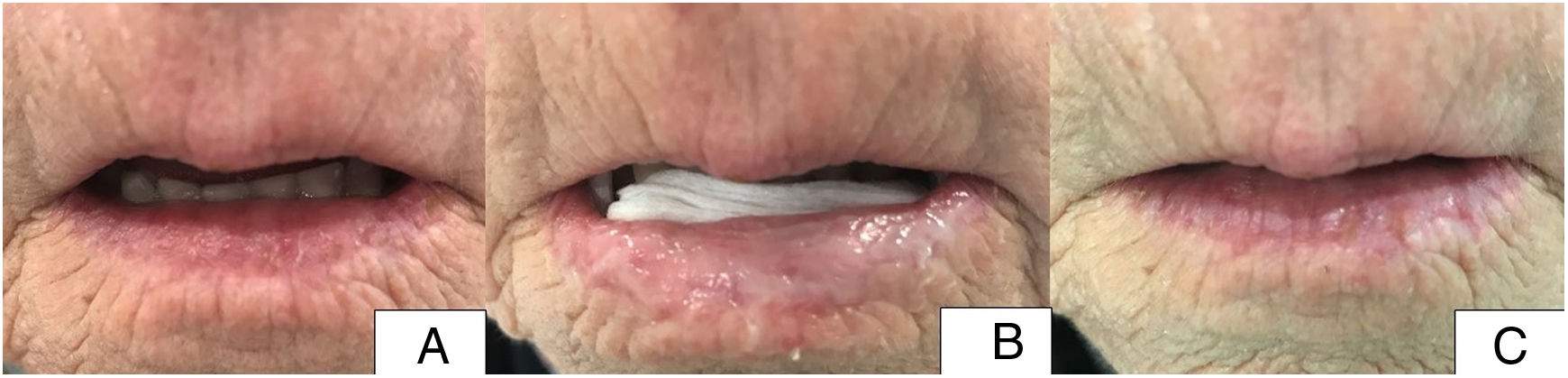
Patient 3. A, Initial state of the patient before treatment, with involvement of 75% of the surface of the lower lip (central region and adjacent lateral areas). B, Image of patient with methyl aminolevulinate cream applied and gauze on the posterior face of the lower lip. C, Image of the patient after 8 weeks of treatment. Complete resolution of the lesions.
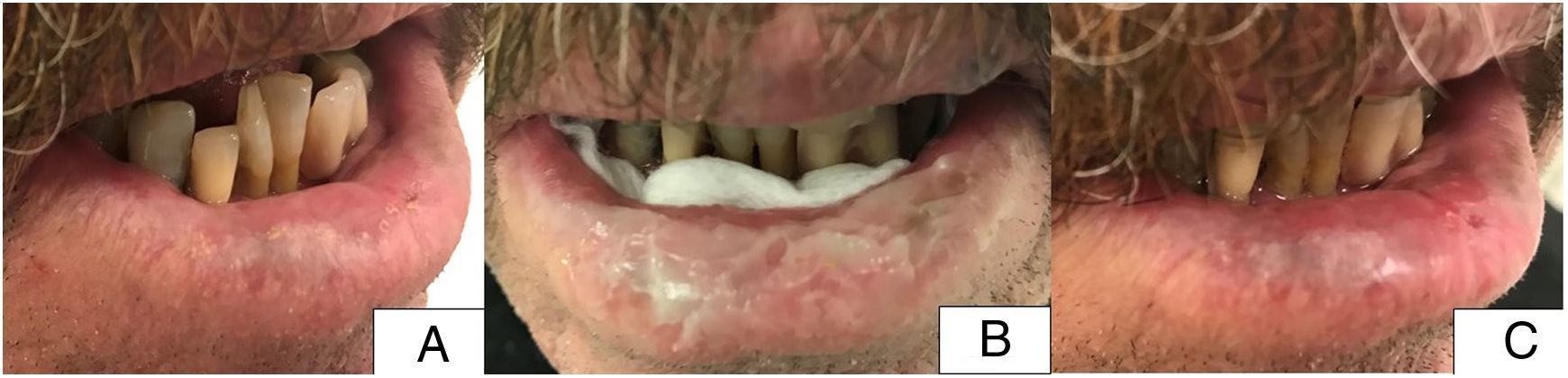
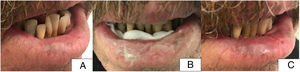
Patient 4. A, Initial situation of the patient before treatment with involvement of 75% of the surface of the lower lip (right lateral and central region). B, Image of patient with methyl aminolevulinate cream applied and gauze on the posterior face of the lower lip. C, Image of the patient after 8 weeks of treatment. Complete resolution of the lesions.
Actinic cheilitis is a premalignant disease with a rate of transformation to squamous cell carcinoma (SCC) of 16.9% and a relative risk of 2.5 for developing this entity.1,2 Furthermore, labial SCC has a 4-fold higher tendency for developing lymph node metastases compared with SCC on the skin.6,7 Chronic exposure to ultraviolet radiation is the main risk factor implicated in the onset of actinic cheilitis, along with smoking and alcohol abuse.3 Several different treatments have been used for actinic cheilitis, such as ablative methods (cryotherapy, CO2 laser treatment), partial surgical resection, or vermilionectomy, and topical treatments such as imiquimod or 5-fluoracyl.3,8 On the other hand, actinic keratoses are the skin equivalent of actinic cheilitis3 and several different treatments similar to those listed above have been tried, although daylight PDT has also been used. This technique consists of a photosensitizing substance (MAL/5-ALA) that is activated by exposure to ambient sunlight (visible light) without the need for prior occlusion or exposure to red light from a lamp as is the case for conventional PDT.4 Daylight PDT has been associated with efficacy rates similar to conventional PDT (clearance rate of 70% to 93% at 3 months after a single session4,5) with much better tolerance as there is no or minimal pain.4 Conventional PDT has also been used in actinic cheilitis (15 previous studies)3 with a mean clinical response of 60.25% and histological clearance of 47.4%.3 Intense pain during treatment was the main side effect, requiring the administration of oral analgesics or local anesthetic.3 Daylight PDT for actinic cheilitis has been used less frequently, and is only mentioned in 2 studies in the literature,8,9 and in a description of 2 cases.10 Fai et al.8 treated 10 patients with actinic cheilitis with daylight PDT using aminolevulinate cream, obtaining total remission of the affected area in 70% of patients after 3 months; this was maintained in 50% of patients at 6 to 12 months of final follow-up. All patients showed partial remission that was maintained until the end of follow-up. In another study, 11 patients were treated, obtaining a cure rate of 91%,9 and 2 isolated case reports with complete clearance after treatment.10 No adverse effects were reported in any cases. Our results are very similar to those described previously in the literature. All patients experienced a reduction in the affected area after treatment, with complete resolution in 67% of patients. These results exceeded those obtained with other medical treatments such as 5-FU (clinical clearance in 30% to 40% of patients)3 and were similar to imiquimod 5% cream3 (40% to 100%). No side effects were detected other than mild discomfort, with the results obtained with the VAS for pain of 0 or 1 (range 0-10). Despite the limited number of patients, given the results obtained and those presented in previous studies, we consider that daylight PDT is a good alternative for treatment of actinic cheilitis. This technique obtains response rates similar to those of conventional PDT, without the associated pain. There is also no need for a PDT lamp, so it can be performed in any center.
FundingThis study did not receive any funding.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Martín-Carrasco P, Sendín-Martín M, Domínguez-Cruz JJ, Bernabeu-Wittel J. Terapia fotodinámica con luz de día en el tratamiento de la queilitis actínica. Actas Dermosifiliogr. 2020;111:883–885.