Eccrine angiomatous hamartoma (EAH) is a rare, benign cutaneous tumor composed of vascular and eccrine elements. It is most commonly diagnosed during the first years of life, although there are reports of cases diagnosed in adults. We report the ultrasound findings of a 46-year-old patient with a left plantar lesion, histopathological diagnosis of which confirmed suspicion of EAH.
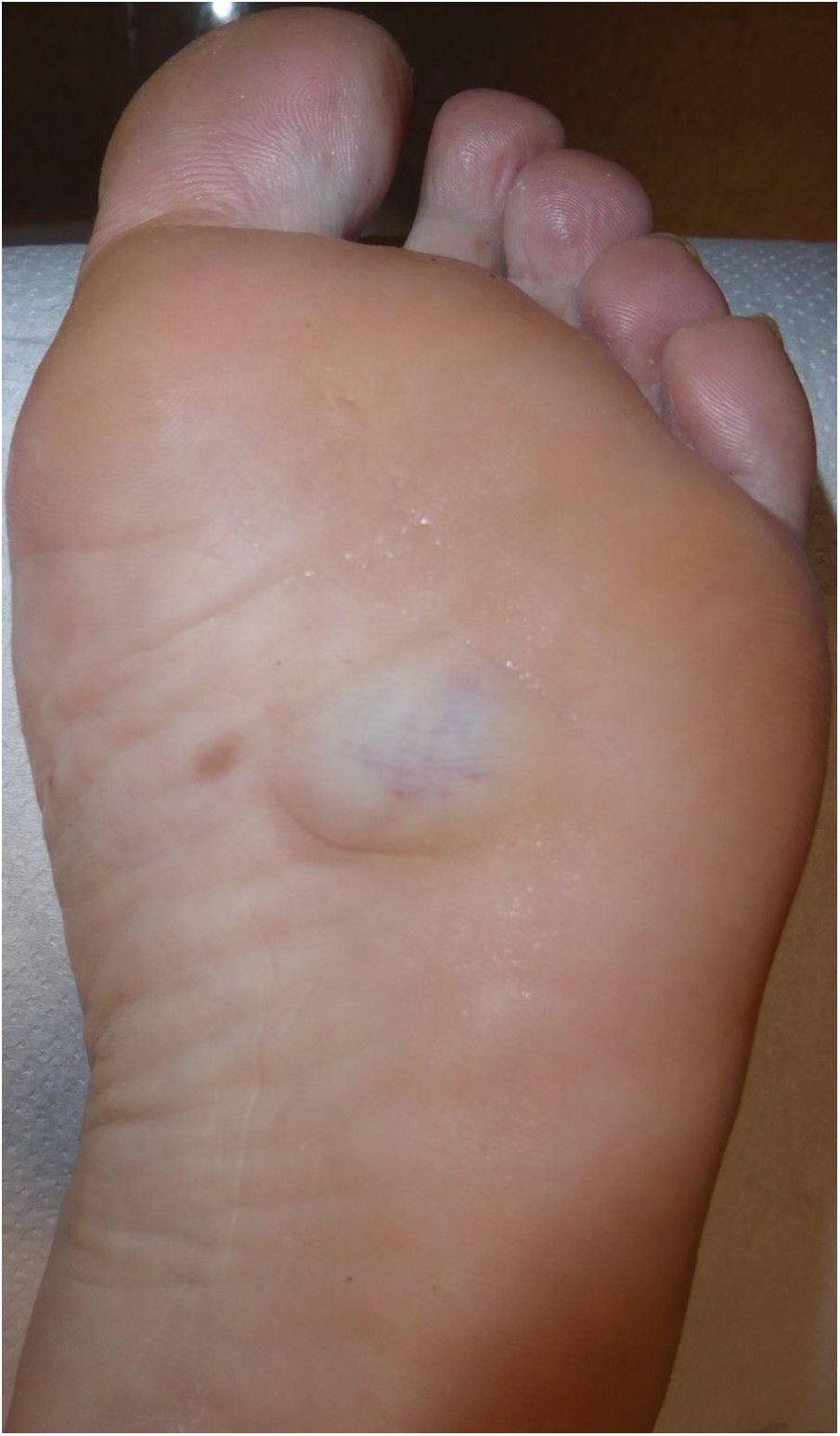
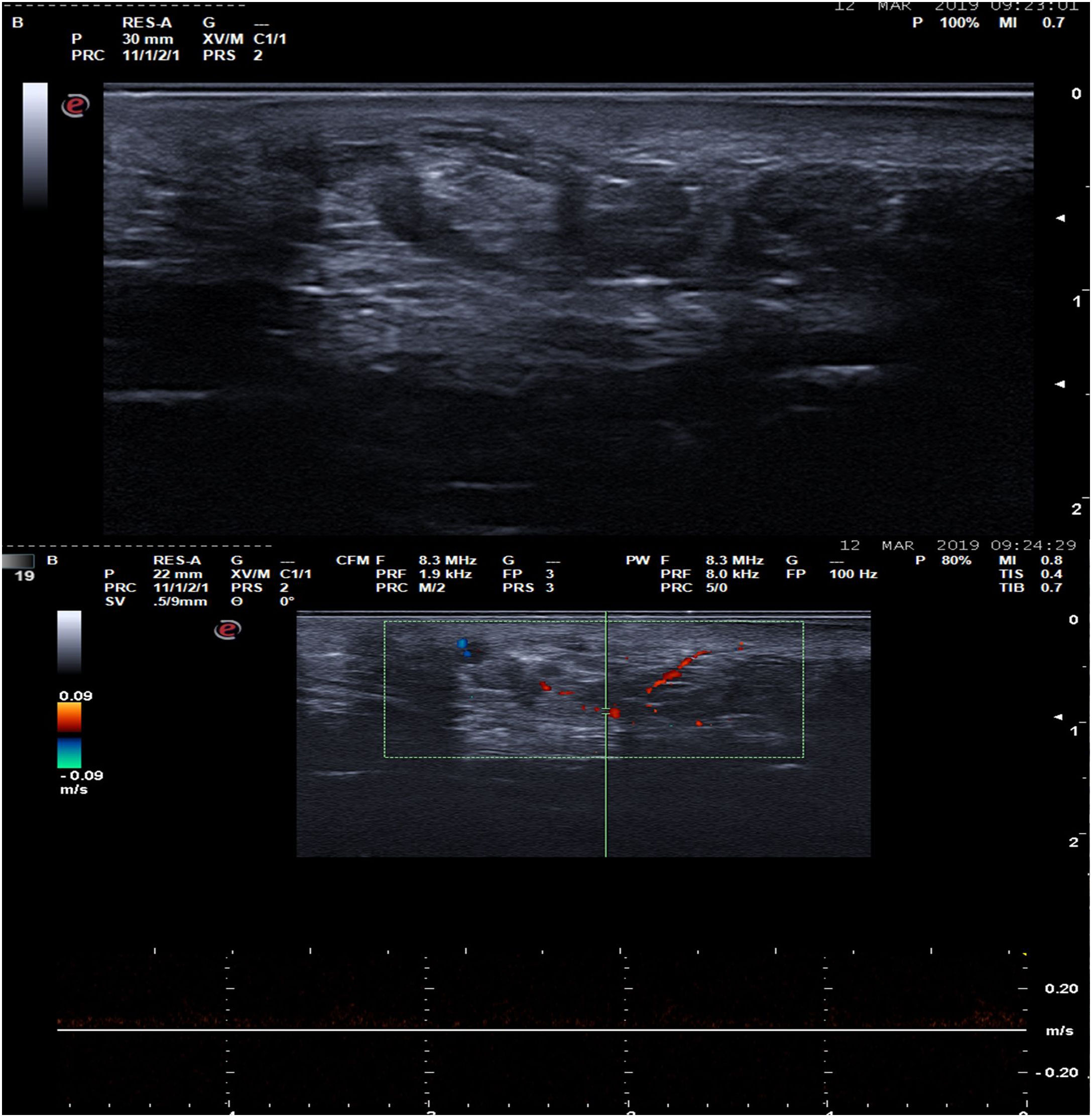
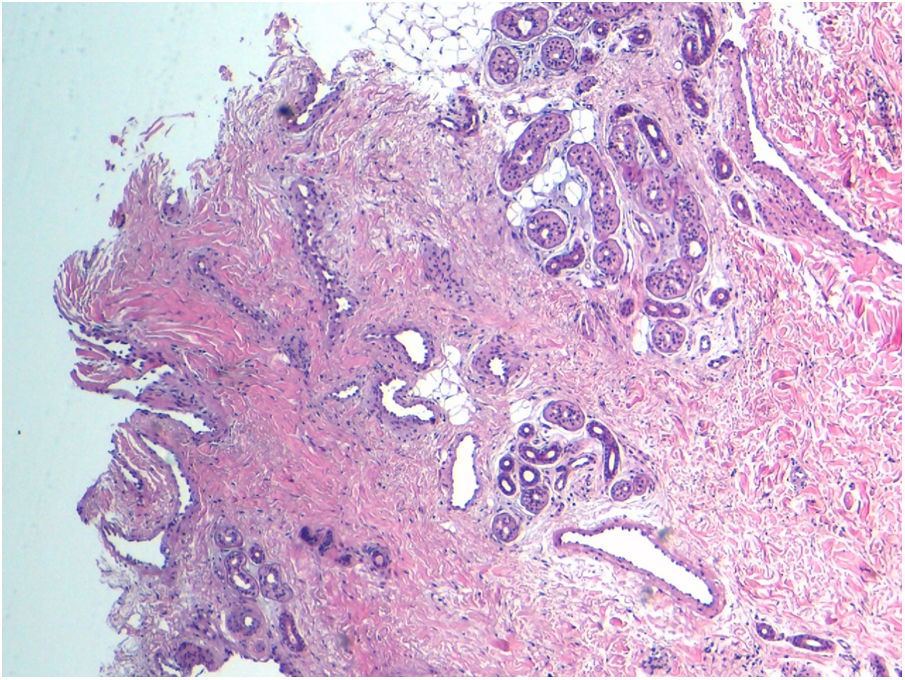
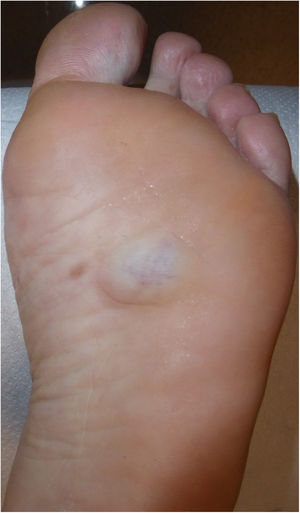
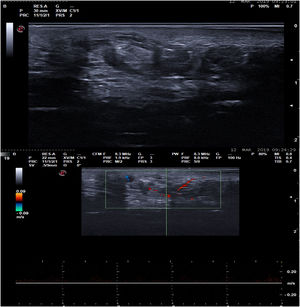
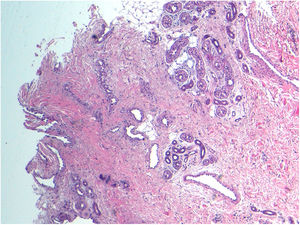
Case DescriptionA 46-year-old woman was seen for mild discomfort in the sole of her left foot when walking. During the anamnesis, she reported a lesion in the midfoot, specifically the plantar support area, that had appeared approximately 10 years earlier. Clinical examination revealed a bluish, rubbery, compressible nodule of approximately 3 cm (Fig. 1). Skin ultrasound with a high-frequency (6–19 MHz) linear probe (Esaote MySix®) revealed a poorly defined dermal–hypodermal lesion. Ultrasound in B mode showed tubular hypoechoic foci with mild posterior acoustic reinforcement and isolated hyperechoic structures (Fig. 2A). Color Doppler mode revealed a moderate increase in intralesional uptake that corresponded to high flow and low resistance in spectral mode (Fig. 2B). Histology showed proliferation of dilated vessels with disorganized distribution at the level of the middle and deep dermis, as well as eccrine gland proliferation and foci of adipose tissue (Fig. 3). Due to the size of the lesion and the possible consequences of excisional surgery, it was decided, in agreement with the patient, not to remove the lesion and to adopt a wait-and-see approach.
A, B-mode ultrasound image showing a poorly delimited, largely hypoechoic lesion containing tubular hypoechoic structures and scattered hyperechoic areas. B, Spectral Doppler ultrasound image, showing focal intralesional hypervascularization corresponding to high-flow, low-resistance vessels.
EAH is a sometimes congenital skin tumor that generally presents during the first years of life. However, adult onset, as in the present case, has been described.1
The etiology and pathogenesis of EAH are poorly understood. It has been proposed that EAH is a consequence of failed interaction between the epithelial and mesenchymal components that leads to abnormal proliferation of vascular and adnexal structures. It has also been postulated that onset in adulthood may be a consequence of repeated microtrauma.2 Appearance of EAH in adulthood may also be due to an absence of symptoms during the first few years and a consequent delay in diagnosis.
EAH usually manifests as a single brownish, blue, or reddish lesion. Multiple lesions can develop, usually in the distal areas of the extremities, palms, and soles.3 Most cases are asymptomatic, although some patients may experience hyperhidrosis and local pain caused by neural infiltration of the eccrine component.4
In addition to the findings of the clinical examination, some recently described dermoscopic findings may be diagnostically useful.5 We decided to perform skin ultrasound because it is a rapid, noninvasive technique that allows visualization of the deep component of lesions, and identification of vascular lesions using color Doppler mode. In our patient, ultrasound revealed a poorly delimited structure at the dermal–hypodermal level with poorly defined hypoechoic areas, which may correspond to intralesional vascular areas. Furthermore, we observed small hyperechoic areas that may correspond to adipose tissue septa interspersed throughout the lesion.
Diagnosis of EAH is clinical, although histopathologic confirmation is necessary. We observed proliferation of eccrine glands, unstructured angiomatous capillaries at the level of the dermis, and variable amounts of adipose tissue.6 The differential diagnosis of EAH includes the following: vascular malformations; tufted angioma (develops during the first 5 years of life and can be associated with hypertrichosis or hyperhidrosis); smooth muscle hamartoma (solitary plaques of childhood onset accompanied by hypertrichosis and hyperpigmentation); and rubber bleb nevus (blue, nodular, depressed lesions).7 However, eccrine nevus is the entity most difficult to differentiate from EAH. Unlike EAH, which is a mixed variant, eccrine nevus consists exclusively of eccrine tissue. Furthermore, while associated hyperhidrosis occurs in almost all cases of eccrine nevus, this clinical finding is observed in only one third of EAH cases.8
Definitive treatment consists of surgical resection, although given the benign nature of the tumor resection is not always necessary, and is usually only considered in cases involving bothersome symptoms such as hyperhidrosis. Other therapeutic alternatives (eg intralesional sclerosing agents, botulinum toxin, or laser) may be useful in certain patients.9
The case presented here underscores the value of imaging the differential diagnosis of EAH.
Please cite this article as: Vilas-Sueiro A, López-Armesto A, Mosquera-Martínez MT, Monteagudo B. Hamartoma angiomatoso ecrino en la edad adulta y sus hallazgos ecográficos. Actas Dermosifiliogr. 2021;112:376–378.