Actinic keratoses (AKs) are common skin lesions associated with an increased risk of developing squamous cell carcinoma. Few studies in Europe have focused on AK prevalence.
AimTo determine the point prevalence of AKs in a dermatology outpatient population in Spain, to describe the clinical characteristics of these lesions and to characterise the profile of AK patients.
MethodsObservational, cross-sectional, multicentre study conducted in 19 hospitals (dermatology outpatient services) around Spain. A total of 204 consecutive patients per hospital who were ≥45 years old were screened for the presence of AKs.
Results3877 patients were assessed and the overall AKs prevalence was 28.6%. Prevalence was significantly higher in men than women (38.4% vs. 20.8%, p<0.0001) and increased with age for both sexes (45.2% in 71–80 years). Scalp and ear lesion locations were significantly more frequent in men (51.9% vs. 2.7% and 16.9% vs. 2.4%, respectively, p<0.0001 both cases) and the cheek, nose and neckline in women (46.3% vs. 34.0% [p<0.0001], 43.0% vs. 24.8% [p<0.0001] and 5.3% vs. 1.8% [p=0.002]). Men showed a significantly higher frequency of ≥2 affected areas than women (42.7% vs. 20.3%, p<0.0001). Among patients with AK lesions, only 65% confirmed that they were the reason for the visit to the clinic.
ConclusionsApproximately a quarter of the dermatology outpatient population in Spain aged ≥45 years old have AKs, with the prevalence rate being highest in men and in older age groups. AK is underdiagnosed and a proactive strategy is needed for the diagnosis and early treatment of these lesions.
Las queratosis actínicas (QA) son lesiones cutáneas comunes asociadas a un mayor riesgo de desarrollar carcinoma de células escamosas. Hay pocos estudios en Europa sobre la prevalencia de QA.
ObjetivosDeterminar la prevalencia de QA en una población de pacientes ambulatorios dermatológicos en España y describir las características clínicas de los pacientes con QA.
MétodosEstudio observacional, transversal, multicéntrico (19 hospitales, servicios de consultas externas de dermatología) en España. Se incluyeron 204 pacientes consecutivamente por centro, edad ≥45 años y se determinó la presencia de QA.
ResultadosSe evaluaron 3.877 pacientes. La prevalencia de QA fue de 28,6% y esta fue más alta en hombres que en mujeres (38,4% vs. 20,8%, p<0,0001), incrementándose con la edad en ambos sexos (45,2%, 71-80 años). Las lesiones en el cuero cabelludo y en la oreja fueron más frecuentes en hombres (51,9% vs. 2,7% y 16,9% vs. 2,4%, respectivamente, p<0,0001 ambos casos) y la mejilla, la nariz y el escote en mujeres (46,3% vs. 34,0% [p<0,0001], 43,0% vs. 24,8% [p<0,0001] y 5,3% vs. 1,8% [p=0,002]). Los hombres presentaron una mayor frecuencia de ≥2 zonas afectadas vs. mujeres (42,7% vs. 20,3%, p<0,0001). Entre los pacientes con QA solo el 65% confirmó que esta era el motivo de la visita.
ConclusionesAproximadamente una cuarta parte de la población ambulatoria de dermatología en España ≥45 años presenta alguna QA, con una prevalencia más alta en los hombres y los grupos de mayor edad. La QA está infradiagnosticada y se requiere de una estrategia proactiva para el diagnóstico precoz y el tratamiento.
Actinic keratoses (AKs) are common skin lesions primarily caused by non-ionizing radiation, in particular ultraviolet light associated with chronic sun exposure. People with AK have an increased risk of developing squamous cell carcinoma (SCC) and other skin malignancies.1 A systematic review showed that the progression rate of AK to invasive SCC was between 0% and 0.075% per lesion-year,2 with a higher rate of progression for immunosuppressed patients.3,4
Studies of AK prevalence in Europe are scarce and reported prevalence rates vary greatly; ranging from 1% to 3% reported in Italy and Germany5,6 to 29% to 49% in men and 24% to 28% in women in Austria and Netherlands, respectively.7,8 This variability is most likely due to differences in methodology, population phototype, and the geographic location of the sample.5–9 Currently, there are no data available on the AK prevalence in Spain and AK is thought to be underdiagnosed due to the asymptomatic nature of the lesions.
The main aim of this study was to determine the prevalence of AK in a Spanish population attending general dermatology outpatient clinics for any reason.
Materials and methodsThis was an observational, cross-sectional, and multicentre study.
Estimating a 15% of AK prevalence in patients aged 45 years or over and an alpha risk of 95% for an accuracy of 1% in bilateral contrast, a sample of 4032 patients was planned according to the protocol.
In order to ensure minimal geographic misrepresentation (and avoid potential climate bias), 19 out of 20 Hospitals with dermatology services were selected (1 centre retired before starting of the study) from the different autonomous communities across the northern, central, southern and Mediterranean areas of Spain.
Each hospital aimed to include 204 Caucasian patients, aged 45 years or older, who consecutively attended a general dermatology outpatient clinic for any reason, at any time from October 2013 to April 2014. Immunosuppressed patients were excluded. Written informed consent was obtained from every participant.
Whole-body examinations were performed by certified dermatologists. Patients were screened for the presence of AK lesions at pre-defined anatomical sites (face, scalp, ears, back of the hands and forearms, neck and others). Standardised interviews regarding personal and medical history were conducted and included the following topics: profession, sun exposure habits, use of artificial light sources, and personal history of non-melanoma skin cancer.
Point prevalence was given as percent values; corresponding 95% confidence intervals (95% CI) were computed by a general method using normal distribution.
Description of qualitative variables was performed using absolute frequencies and percentages. Standard descriptive statistics such as mean and standard deviation (SD) were also calculated. Qualitative variables were analysed by the Chi-square test or the Fisher exact test, as appropriate, and quantitative variables were analysed using the t-test or the Mann–Whitney test. Values of p<0.05 were considered statistically significant. No imputations to missing data were performed. Statistical analysis was performed using IBM SPSS statistics V.19 (SPSS, an IBM company, Chicago, Illinois, USA).
The study was conducted in accordance with the Declaration of Helsinki and local laws and regulations. All patients provided written informed consent before study entry. The study was approved by the Ethical Committee of Hospital Universitari Germans Trias i Pujol.
ResultsA total of 3877 patients were recruited and all of them were included. Of the 20 hospitals selected, 19 participated in the study (one hospital retired from the study without including any patients). Patients’ mean (SD) age was 66.1 (12.2) years and, 55.6% (n=2156) were women. The presence of AK lesions was the reason for consultation for 748 (19.3%) patients, with the remaining 3129 (80.7%) patients citing “other reasons” for the consultation (Table 1).
Demographical and clinical characteristics of the total population.
| Total population (n=3877) | |
|---|---|
| Sex (female), n (%) | 2156 (55.6%) |
| Age (years), mean (SD) | 66.1 (12.2) |
| Median (min, max) | 66 (45; 100) |
| Reason for consultation, n (%) | |
| AK | 748 (19.3%) |
| Other reasonsa | 3129 (80.7%) |
| High solar exposure due to profession,cn (%) | 879 (22.7%) |
| High solar exposure by occupation,dn (%) | |
| Farmers, ranchers, and fishermen | 404 (10.4%) |
| Artisans, builders | 167 (4.3%) |
| Elementary occupations | 154 (4.0%) |
| High solar exposure due to recreational activities,bn (%) | 1024 (26.4%) |
AK, actinic keratosis; SD, standard deviation.
High recreational sun exposure was considered when the patient regularly participates in outdoor recreational activities year round.
The percentage of patients was calculated among the total of AK patients with other reasons for consultation (n=390): cutaneous carcinomas (n=153, 39.2%), melanoma (n=12, 3.1%), inflammatory dermatitis (n=45, 11.5%), benign pigmented tumours (n=21, 5.4%), other benign tumours (n=90, 23.1%), cutaneous infections (n=20, 5.1%), miscellany (n=23, 5.6%), adnexal diseases (n=15, 3.8%), pruritus (n=8, 2.1%), and mucosal disease (n=4, 1.0%).
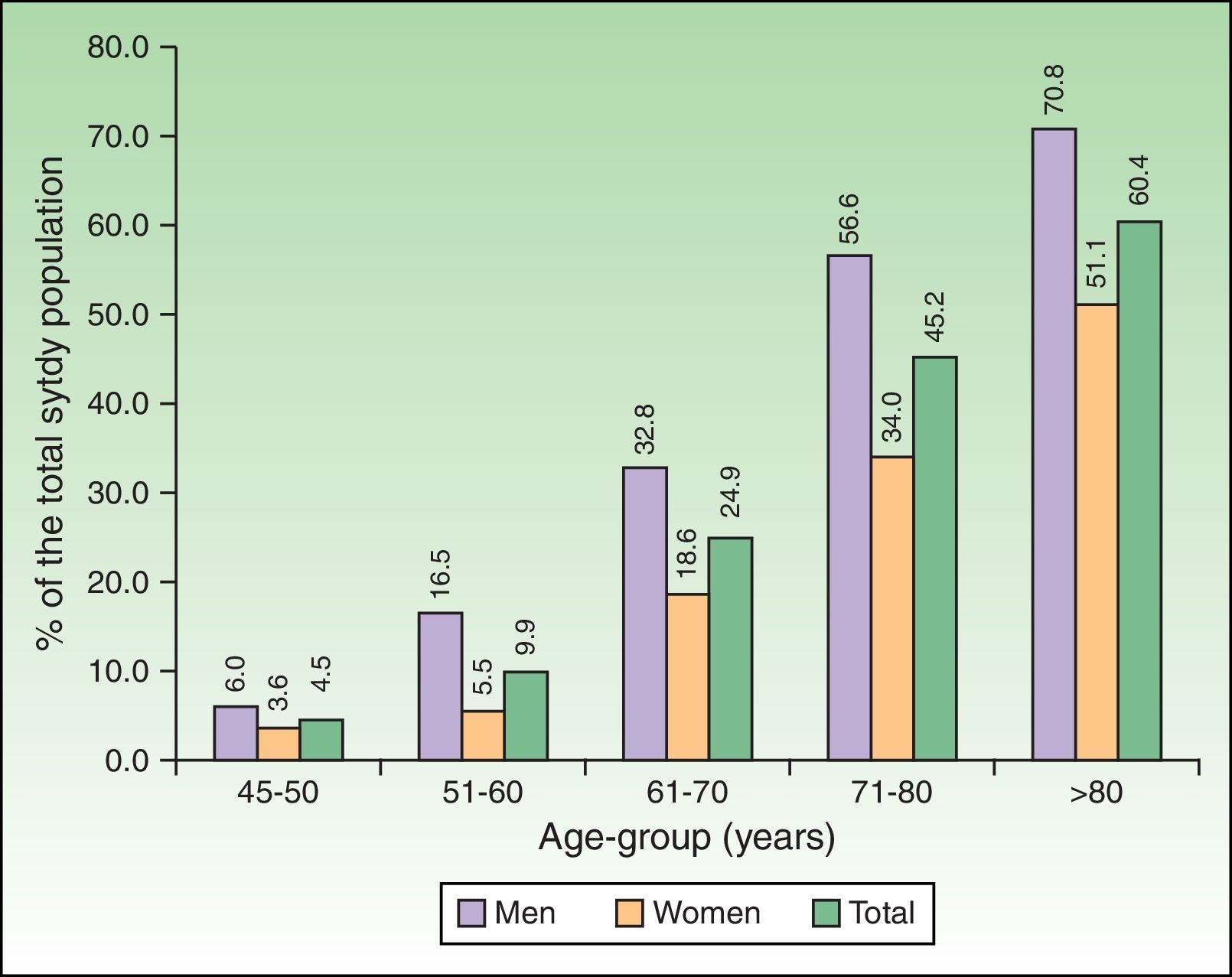
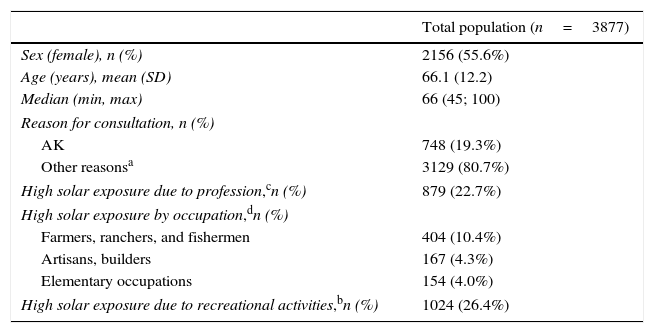
Among the 3877 patients included, 1110 had confirmed AK (28.6%, 95% CI 27.2–30.1). This point prevalence was significantly higher in men than women (38.4%, 95% CI 36.1–40.7 vs. 20.8%, 95% CI 19.1–22.6, p<0.0001) and increased with age (4.5% in the age group 45–50 years old to 60.4% in those over 80 years old) [Fig. 1].
The distribution of AK according to geographical distribution showed the highest prevalence in the Mediterranean and southern areas of Spain (31.4% and 28.1%, respectively), compared to the northern and central areas (27.5% and 24.9%, respectively).
A positive correlation between age group and AK prevalence was observed (r=0.985, p=0.01), and was significantly higher for men compared to women in all age groups (p<0.0001) except for patients between 45 and 50 years old (Fig. 1).
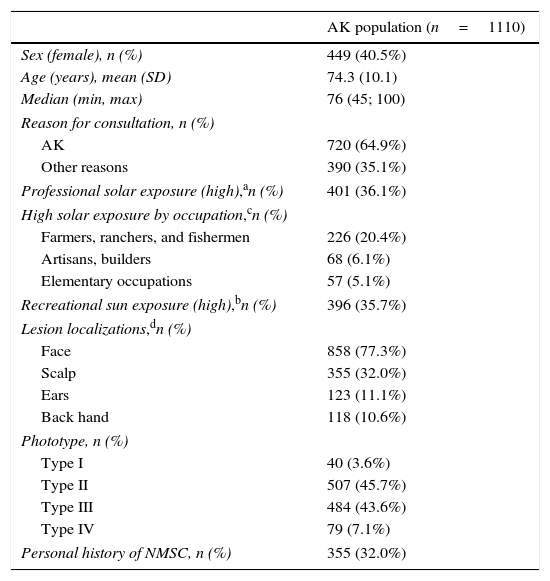
Patients with confirmed AK had a mean age of 74.3 (10.1) years and 59.5% were male. More than one-third of patients had high recreational sun exposure (35.7%). The most frequent phototypes were II and III (45.7% and 43.6%, respectively) and 32.0% had a personal history of non-melanoma skin cancer. Thirty-five percent of patients were unaware of having AK and attended the dermatology consultation for other reasons (Table 2).
Demographical and clinical characteristics of patients with AK.
| AK population (n=1110) | |
|---|---|
| Sex (female), n (%) | 449 (40.5%) |
| Age (years), mean (SD) | 74.3 (10.1) |
| Median (min, max) | 76 (45; 100) |
| Reason for consultation, n (%) | |
| AK | 720 (64.9%) |
| Other reasons | 390 (35.1%) |
| Professional solar exposure (high),an (%) | 401 (36.1%) |
| High solar exposure by occupation,cn (%) | |
| Farmers, ranchers, and fishermen | 226 (20.4%) |
| Artisans, builders | 68 (6.1%) |
| Elementary occupations | 57 (5.1%) |
| Recreational sun exposure (high),bn (%) | 396 (35.7%) |
| Lesion localizations,dn (%) | |
| Face | 858 (77.3%) |
| Scalp | 355 (32.0%) |
| Ears | 123 (11.1%) |
| Back hand | 118 (10.6%) |
| Phototype, n (%) | |
| Type I | 40 (3.6%) |
| Type II | 507 (45.7%) |
| Type III | 484 (43.6%) |
| Type IV | 79 (7.1%) |
| Personal history of NMSC, n (%) | 355 (32.0%) |
AK, actinic keratosis; SD, standard deviation; NMSC, non-melanoma skin cancer.
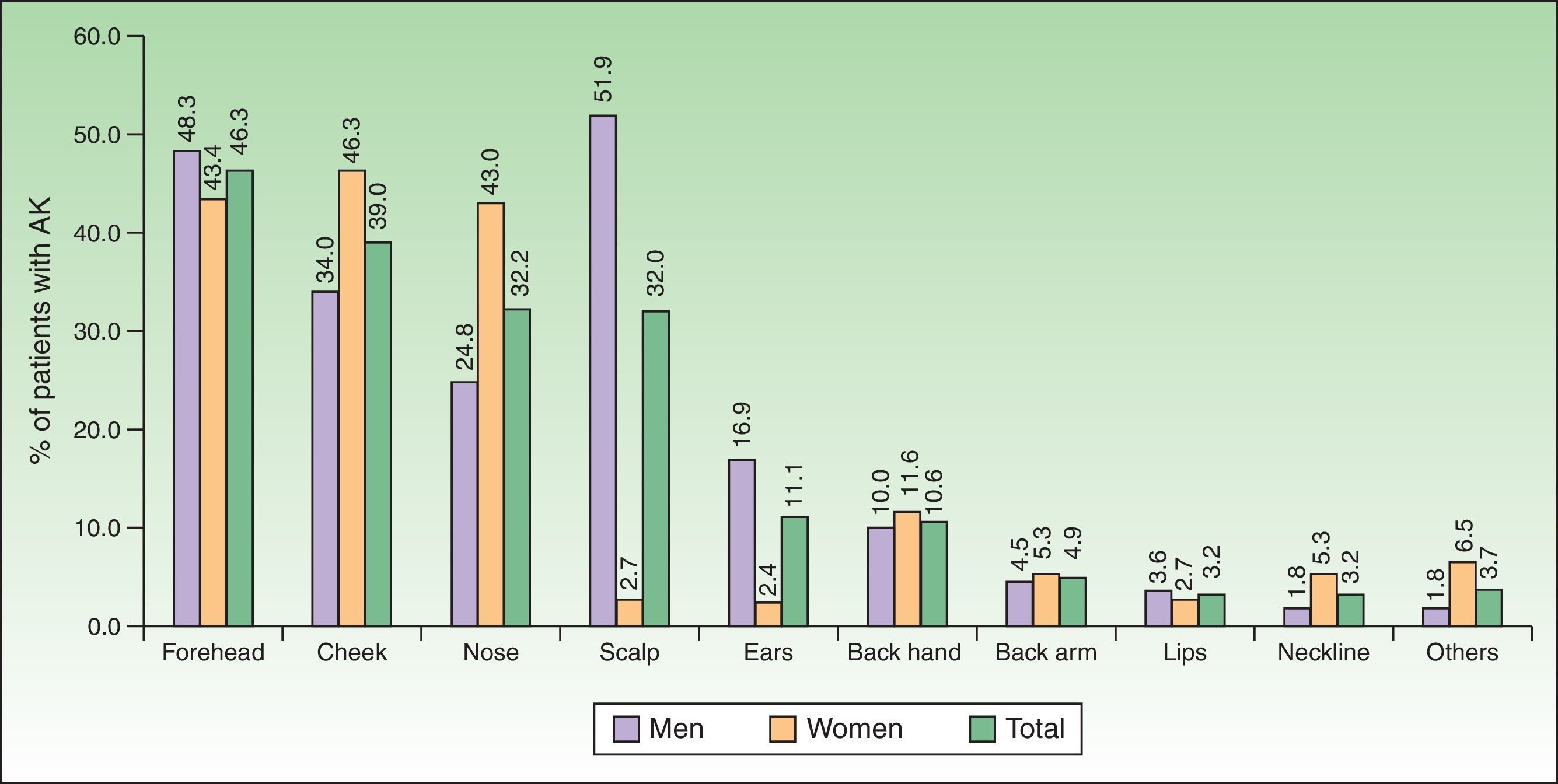
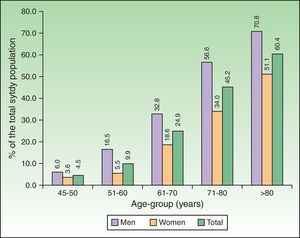
The frequency of AK according to anatomical location was most common on the face (77.3%, with the forehead being the most frequent [46.3%]), followed by the scalp (32.0%). Comparisons by sex according to location showed significant differences (men vs. women) for the scalp (51.9% vs. 2.7%, p<0.0001), and ears (16.9% vs. 2.4%, p<0.0001). By contrast, nose and cheek were significantly more affected in women compared to men (43.0% vs. 24.8%, and 46.3% vs. 34.0%, p<0.0001 in both cases), as was the neckline (5.3% vs.1.8%, p=0.0020) [Fig. 2].
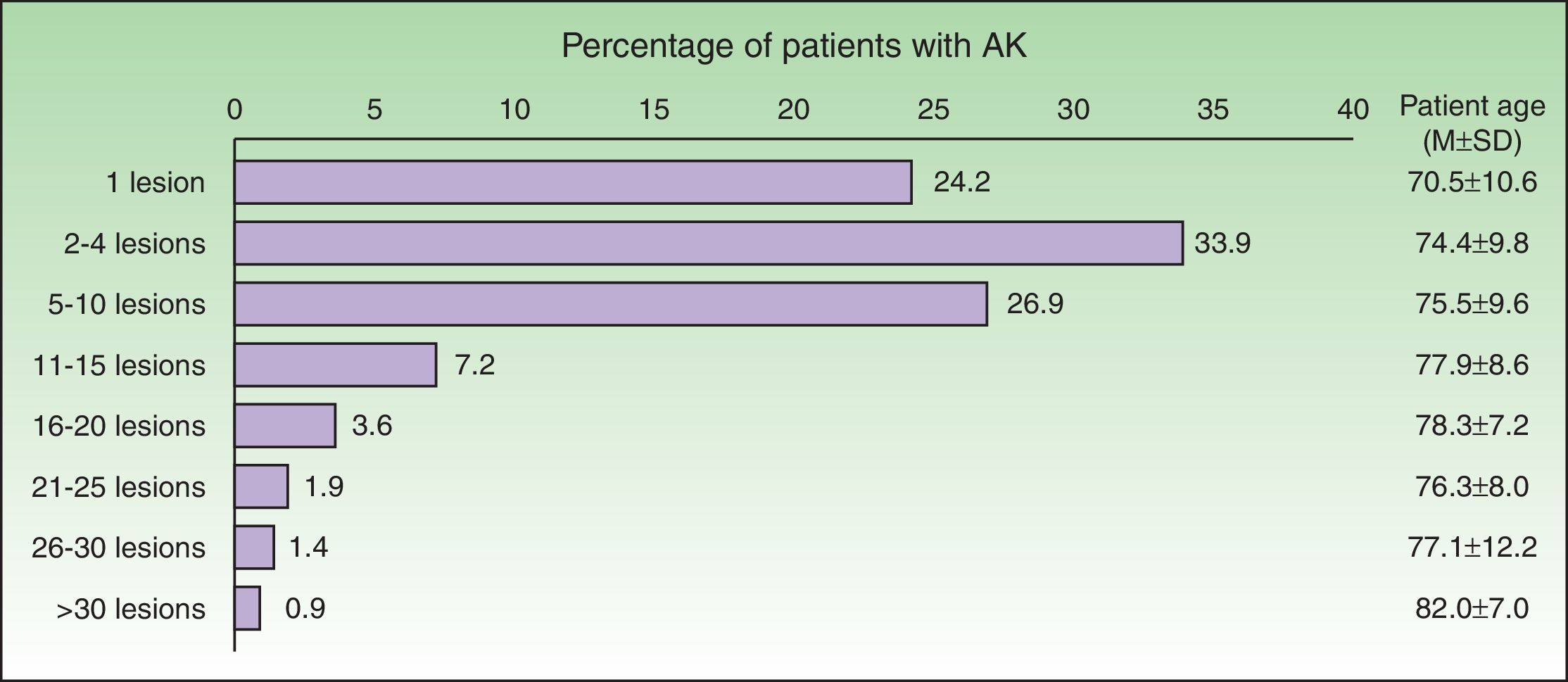
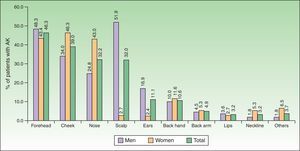
Extent of diseaseOnly one out of four patients with AK presented with a single lesion. Thirty-four percent of patients had 2–4 lesions, and 26.9% 5–10 lesions. The mean age of patients according to the number of lesions was statistically significant, that is, as age increased, the number of lesions significantly increased (p<0.0001) [Fig. 3].
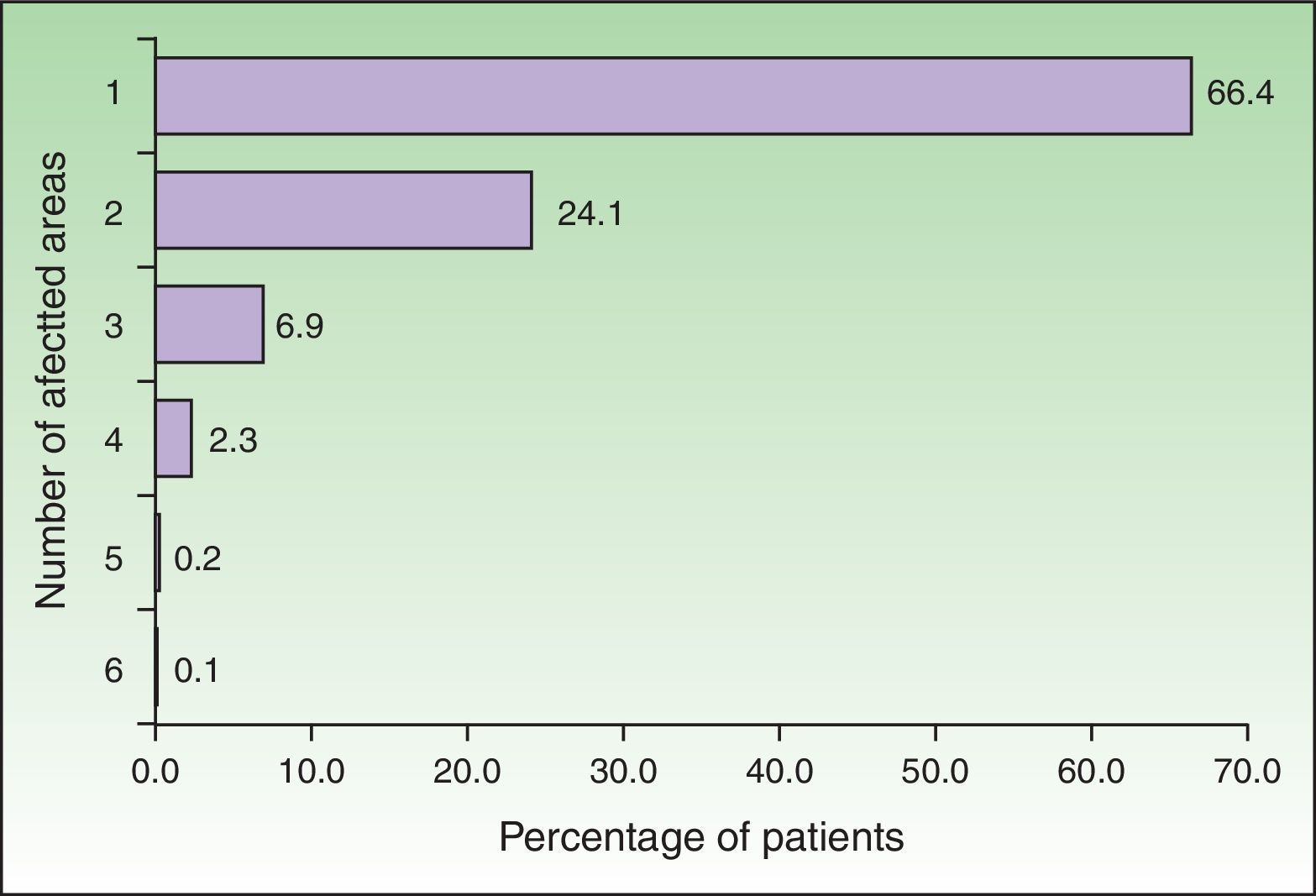
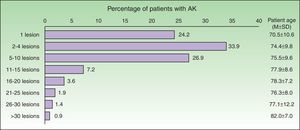
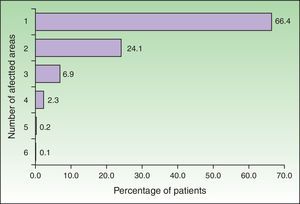
The number of affected areas was statistically associated with age (p<0.0001) [Fig. 4]. Men had a significant higher frequency of having two or more affected areas compared to women (42.7% vs. 20.3%, p<0.0001).
DiscussionIn this study the overall prevalence of AK was 28.6% in a dermatology outpatient population aged ≥45 years old (38.4% in men and 20.8% in women). These results reflect similar overall AK prevalence rates from other recent studies conducted in Netherlands and Austria (2061 inhabitants and 4449 dermatology patients, respectively) that showed a prevalence of 37.5% (49.0% in men and 28.1% in women, in patients >50 years old) and 31.0% (39.2% in men and 24.3% in women, aged ≥30), respectively.7,8 By contrast, several studies have found lower prevalence rates within other study populations. For example, a study in the North of England found an AK prevalence of 15.4% in men and 5.9% in women, in a sample of 968 subjects >40 years attending outpatient clinics.9 Furthermore, large studies in Germany (determined in a cohort of 90,800 employees from 300 companies) and Italy (which included a total of 12,483 subjects selected from electoral rolls) displayed much a lower AK prevalence of 2.7% (3.9% in men and 1.5% in women, patients aged 16–70 years) and 1.4% (1.5% in men and 1.4% in women, in patients aged ≥45), respectively.5,6 The low AK prevalence observed in Germany may be underestimated due to the age range of the selected population – employees aged 16–70 years old that did not include retirees, where AK is most prevalent, and included young people, in whom AK is very rare. More surprising is the low prevalence reported in Italy, given its similar climate to Spain. One possible explanation for the disparity results presented here and those of the Italian study is the staff who assessed the AK lesions; in this study the assessment was performed by certified dermatologists, whereas the Italian study assessments were performed by trained interviewers (2-h teaching session) who conducted a face-to-face interview at the subjects house.
Taken together, the results reported here and in other European studies suggest a highly variable prevalence that may be enhanced by subject selection which, among other factors, included different age groups. Moreover, in some studies the subject selection involved those attending dermatology services, while in other studies subjects were selected from electoral rolls, insurance companies’ data, or districts. In addition, the examination procedure in some studies was performed by dermatologists while in others it was performed by trained interviewers. Finally, the geographical location with different levels of UV radiation and different phototypes could also be a factor which contributed to the heterogeneity of the prevalence results reported.
In this study the prevalence of AK was observed to increase with age for both sexes, reaching 60.4% of patients older than 80. Similar observations were previously reported in other studies.6,7,9 Moreover, in line with previous results, our data showed a higher prevalence of AK in men (38.4%) compared to women (20.8%).5–10 A possible explanation for this higher AK prevalence in men could be an increased occupational lifetime sun exposure associated with outdoor work. Studies conducted in Austria and the UK demonstrated higher AK prevalence rates in outdoor workers.11,12 Consistent with this, Harvey et al.10 also found cumulative sun exposure to be a significant risk factor associated to AK. Furthermore, a presumed lower-compliance with sun protection measures in men, differing hair coverage of the scalp and ears, and a much higher prevalence of baldness in men could also contribute to these sex differences.
With regard to anatomical location, in this study AK lesions were correlated with the most intense chronic UV light exposure such as the forehead and scalp. The most frequently reported locations in men were the scalp and ears whereas for women the nose, cheek and neckline were more common. This data agrees with previous work which reported that the scalp was the most frequent location in bald men vs. women (47.5% in men vs. 0.0% in women8). The difference in the frequency of lesions on the ears in men compared to women was also consistent with previous data from Youl et al.13 and Eder et al.7 who reported that ears were 3.4 and 5.8 times, respectively, more commonly affected in men than women with AK. In this study, it should be noted that the frequency of lesions in the nose, cheek and neckline was significantly higher in women than in men. These results are in agreement with previous studies that found that lesions on the face were more frequent in women than in men and scalp and ears were more frequent in men versus women.13 These differences in AK locations could be explained as areas like scalp and ears are more frequently uncovered in men than in women.
In relation to the number of lesions, an increase with age was observed. Patients with only one lesion had a mean age of 71 years of age, whereas in those patients with more than 30 lesions a mean of 82 years of age was recorded. These results are in accordance with those reported by Flohil et al.8 which showed that age was significantly associated with extensive actinic damage (≥10 AKs). Moreover, it was observed that the number of affected areas increases with age, as previously reported.7
It should be pointed out that 35% of patients with AK lesions ignored their presence. This shows that AK is an underdiagnosed disease and that a proactive strategy is required by the physician for the diagnosis and treatment of these lesions.
This study has some limitations that should be noted. Firstly, the population of this study was restricted to patients visiting dermatology outpatient clinics, which may overestimate the number of patients with AK and might be not representative for the general population. Secondly, AK can be similar to SCC which may in some cases lead to misclassification. Nevertheless, some studies have showed a high predictive value for clinical AK diagnosis.14 Thirdly, AK prevalence was determined using a cross-section of participants attending an outpatient clinic, thus it was unknown whether participants were previously treated for AK, which could have resulted in an underestimation of the AK prevalence.
To the best of our knowledge, this is the first study to estimate of the prevalence of AK in adult dermatology outpatients in Spain. Nearly a quarter of 45-year-old patients or older were found to be affected with AK and this proportion increased with age. Knowledge about characteristics of patients with AK, geographic distribution, and AK locations will help to improve prevention, early detection and contribute to the development of effective treatment strategies to optimise clearance of AK lesions. Furthermore, early detection may have further downstream benefit in developing therapeutic interventions to prevent progression to invasive cutaneous neoplasia. Finally, it should be noted that almost than one-third of patients in this study have ignored the presence of these lesions, which suggest that AK is underdiagnosed and an early proactive detection and early treatment of AK lesions is needed in order to prevent the further development of invasive SCC.
Ethical disclosureProtection of human and animal subjectsThe authors declare that the procedures followed were in accordance with the regulations of the relevant clinical research ethics committee and with those of the Code of Ethics of the World Medical Association (Declaration of Helsinki).
Confidentiality of dataThe authors declare that they have followed the protocols of their work centre on the publication of patient data.
Right to privacy and informed consentThe authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
FundingThis study was funded by Almirall S.A.
Conflict of interestsCarlos Ferrandiz has received honoraria for lectures and/or consultancy Almirall, Leo Pharma and Spherium Biomed. Maria Jose Plazas is employed by Almirall. The other authors have no conflict of interest.
We would like to thank to all the investigators of the EPIQA study group (in alphabetical order): Albares Tendero MP, Alcántara Reifs CM, Alfaro Rubio A, Alonso San Pablo MT, Bassas Freixas P, Blanco Barrios S, Blanes Martínez MM, Botella Estrada R, Brufau Redondo C, Castellanos González M, Curto Barredo L, De La Corte Sánchez IS, De La Cueva Dobao P, Del Prado Sanz ME, Eiris Salvado N, El-Khalili Murjan BA, Escutia Muñoz B, Fernández López E, Ferrándiz Foraster C, Ferrándiz-Pulido L, Ferrándiz-Pulido C, Figueroa Silva O, Fuente González MJ, Galiano Mejías S, García Acebes CR, García Martínez FJ, García Rodiño S, García-Melgares Linares ML, García-Patos V, Gilaberte Calzada Y, Gómez Bernal SM, Gómez López A, Gómez Sanchez ME, Gonzalez De Arriba M, Heras Mendaza F, Hernández-Gil Bordallo A, Hernández-Gil Sánchez J, Hilari Carbonell H, Hueso Gabriel L, Lera Imbuluzqueta JM, López Aventín D, Marín Corbalán N, Martorell Calatayud A, Mateo Suárez S, Navarro Mira M, Ojeda Vila, T Pérez Caballero JA, Pérez García LJ, Pujol R, Ramírez Andreo A, Ramón Sapena R, Redondo Bellón P, Rodríguez Martín AM, Román Curto C, Romo Melgar A, Roncero Riesco M, Ruiz De Casas A, Ruiz Martínez MD, Salas García T, Salido Vallejo R, Sánchez Aguilar MD, Santos Duran JC, Segurado Rodríguez MA, Soria Martínez C, Valdés Pineda FJ, Vargas Díez E, Vázques Veigas HA, Vázquez Osorio I, Vizán de Uña MC, Yuste Chaves M.